Insurance (general): India
This article has been sourced from an authoritative, official readers who wish to update or add further details can do so on a ‘Part II’ of this article. |
The source of portions of this article
INDIA 2012
A REFERENCE ANNUAL
Compiled by
RESEARCH, REFERENCE AND TRAINING DIVISION
PUBLICATIONS DIVISION
MINISTRY OF INFORMATION AND BROADCASTING
GOVERNMENT OF INDIA
Agriculture insurance
Agriculture Insurance Company of India Ltd (AIC)
A separate organization for agriculture insurance viz. Agriculture Insurance Company of India Ltd. (AIC) was incorporated under the Companies Act, 1956 on 20 December, 2002 with the capital participation from General Insurance Corporation of India (GIC), four public sector general insurance companies viz., (i) National Insurance Company Ltd., (ii) New India Assurance Company Ltd., (iii) Oriental Insurance Company Ltd., and (iv) United India Insurance Company Ltd. and NABARD. The promoter’s subscription to the paid-up capital is 35 per cent by GIC, 30 per cent by NABARD and 8.75 per cent each by the four public sector general insurance companies.
The authorised capital of the AIC is Rs 1,600 crore, while the initial paid-up capital is Rs 200 crore. The company had commenced business from 1 April 2003. While AICIL underwrote crop insurance to begin with, it has covered other allied rural/agricultural risks also. National Agriculture Insurance Scheme (NAIS) which was being implemented by the General Insurance Corporation of India (GIC) was transferred to the AICIL, in addition to NAIS. AICIL is also implementing Weather Based Crop Insurance Scheme (WBCIS).
Appreciating the importance of agriciulture insurance the Government of India while approving the National Policy for Farmers 2007, has taken into account the recommendations of National Commission on Farmers for inclusion of crop insurance as a part of a comprehensive approach towards development and sustenance of the farm sector.
National Agricultural Insurance Scheme (NAIS)
NAIS was implemented from Rabi 1999-2000 season replacing Comprehensive Crop Insurance Scheme (CCIS). The Scheme is being implemented by the Agriculture Insurance Company of India Ltd. on behalf of Ministry of Agriculture. The main objective of the Scheme is to protect the farmers against the losses suffered by them due to crop failure on account of natural calamities, such as drought, food, hailstorm, cyclone, fire, pest/diseases, etc, so as to restore their credit worthiness for the ensuring seasons.
The Scheme is available to all the farmers both, loanee and non loanee irrespective of the size of their holding. The Scheme envisages coverage of all crops including cereals, millets, pulses, oilseeds and annual commercial and horticulture crops in respect of which past yield data of 10 years, is available.
At present, 70 different Food and Oilseed crops are covered during Kharif and Rabi seasons. Sugarcane, Potato, Ginger, Onion, Turmeric, Chilly, Jute, Tapioca, Banana, Pineapple, Brinjal, Coriander, Cumin, Fennel, French Bean, Garlic, Isabgol, Fenugreek and Tomato have been brought under insurance coverage among the annual commercial/horticultural crops.
As per the provisions of National Agriculture Insurance Scheme, the flat premium rates are 3.5 per cent for Bajra and Oilseeds, 2.5 per cent for other Kharif crops; 1.5 per cent for Wheat, and 2 per cent for other Rabi crops. In case actuarial rates are less than prescribed flat premium rates, the lower rate is applicable for food crops and oilseeds.
In case of annual commercial and horticulture crops, actuarial rates are charged. At present, 10 per cent subsidy in premium is allowed for small and marginal farmers, shared equally by Central and State government.
However, some State and Union Territory governments are also providing higher subsidy to small and marginal farmers and subsidy to other farmers. The Scheme operates on the basis of 'Area Approach' for widespread calamities. The unit of insurance may be Gram Panchayat, Mandal, Hobli, Circle, Phirka, Block, Taluka etc., to be decided by the respective State/UT Government.
At present, 25 States and 2 Union Territories are implementing the Scheme. Some of the states have notified lower unit of insurance such as village. Till kharif 2009 season, 15.23 crore farmers were covered with area insurance of 23.63 crore hectares, sum insured of Rs 174910 crore, compensating 4.28 crore farmers with claim amount of Rs 18725.27 crore since the inception of the scheme.
Weather Based Crop Insurance Scheme (WBCIS)
From the season Kharif 2007-08, AIC has started implementing WBCis as a pilot risk mitigation scheme as an alternative to NAIS. WBCIS is a parametric insurance product designed to provide insurance protection to the cultivator against adverse weather incidence during the cultivation period, such as deficit and excess rainfall, frost, heat (temperature), relative humidity, wind speed etc. which are deemed to adversely impact the crop yield.
Crops and Reference Unit Areas (RUA) are notified before the commencement of the season by the State Governments. Each RUA is linked to a Reference Weather Station (RWS), on the basis of which payout/claims are processed. The payouts are made on the basis to adverse variations in the current season's weather parameters as measured at Reference Weather Station (RWS). Claim under WBCIS is area-based and automatic. Insured cultivators are not needed to intimate losses or lodge claims to the insurers.
During Kharif 2007 season, the scheme was implemented in Karnataka covering 70 Hoblis. During Rabi 2007-08 season, the Scheme was implemented in the State of Rajasthan, Chattisgarh, Madhya Pradesh and Bihar.
During the Kharif 2008 season, the Scheme was implemented in 10 States, namely, Madhya Pradesh, Haryana, Punjab, Bihar, Rajasthan, Jharkhand, Maharashtra, Karnataka, Orissa and Tamilnadu. During Rabi 2008-09 season, the Scheme was again implemented in 10 States, namely, Haryana, Bihar, Rajasthan, Jharkhand, Karnataka, Tamil Nadu, Kerala, West Bengal, Chhattisgarh and Himachal Pradesh.
During Kharif 2009 season, the Scheme was implemented in 13 States, namely, Madhya Pradesh, Haryana, Bihar, Rajasthan, Jharkhand, Maharashtra, Karnataka, Orissa, Tamilnadu, Gujarat, West Bengal, Andhra Pradesh and Kerala.
During the Rabi 2009-10 season, the Scheme was again implemented in 11 States, namely, Haryana, Bihar, Madhya Pradesh, Rajasthan, Jharkhand, Karnataka, Tamilnadu, Kerala, West Bengal, Andhra Pradesh and Himachal Pradesh. The coverage so far under WBCIS is shown in the table below:
Besides the above, AIC has designed and implemented various crop insurance
products to cater to the diverse needs of farming community of India such as Apple
Insurance, Cardamon Insurance, Rubber Insurance, etc.
Pradhan Mantri Fasal Bima Yojana (PMBFY)
See Farmers, cultivators and their issues
Successive governments have come out with various schemes to cover farmers against crop loss during disaster or extreme weather events, but the relief for farmers remains patchy . Two reports released on Friday -one by the Comptroller and Auditor General (CAG) and the other by private think-tank Centre for Science and Environment (CSE) -indicate the steep challenges to crop insurance schemes.
Though the new scheme, launched last year, is much better than previous crop insurance schemes (1985-2015) in terms of minimising burden of premium on farmers, expanding the coverage of risks and adopting quicker method of payment, its flawed implementation is a major cause of concern, says CSE.
The CAG has slammed the poor implementation of crop insurance schemes in 2011-16, saying funds to the tune of over Rs 3,622 crore were released to private insurers without verification. In its report, it noted that both central and state governments incurred an expenditure of over Rs 32,606 crore towards payment of premium subsidy and claim liabilities during the five year period.
The CAG report examined the implementation of the crop insurance schemes -NAIS (National Agricultural Insurance Scheme), its modified version MNAIS and Weather Based Crop Insurance Scheme (WBCIS) -through 2015-16. These schemes, however, now have been replaced with new Pradhan Mantri Fasal Bima Yojan (PMFBY) from 2016 kharif season.While the CAG in its report, tabled in Parliament, also figured out how the previous schemes had failed on various counts during 1985-2015 period, the CSE analysed the ground situation on implementation of the Narendra Modi government's ambitious PMFBY and noted several loopholes.
Based on its field study in Haryana, Tamil Nadu and Uttar Pradesh and engagement with farmers, insurance companies and government departments, the CSE noted that the PMFBY mainly remains a scheme for loanee farmers it means farmers who take loans from banks are mandatorily required to take insurance.
“Like previous crop insurance schemes, the PMFBY fails to cover share-croppers and tenant farmers“, said the CSE while listing the loopholes of the new scheme. Even the CAG pointed out this flaw of previous schemes and recommended that the government should make efforts to bring more and more non-lonee farmers under the new scheme.
“The PMFBY is a far superior scheme than the previous agricultural insurance schemes. However, at the state level, its vision is diluted and at the district level, its implementation is seriously compromised. The PMFBY is a classic case of poor implementation of a good scheme“, said the CSE's deputy director general Chandra Bhushan.
1985-2018: highlights
Of the various crop insurance schemes at the national level since 1985, the Pradhan Mantri Fasal Bima Yojana (PMFBY) is the most ambitious risk mitigation programme for farmers. The yield-based National Agriculture Insurance Scheme (NAIS) was the most widely implemented scheme. The present government held a comprehensive review and extensive consultations to close loopholes before a national level rollout in April 2016.
The scheme has been implemented over five seasons now and the scale of finance in each district for each crop forms the basis of calculation of sum insured. This roughly corresponds to cost incurred and gives farmers adequate financial protection without any reduction due to capping in earlier scheme. This sum insured has doubled. The average sum insured, which was Rs 22,000 per hectare, is now Rs 40,000.
The earlier NAIS was based on the trust model where government collected a token premium from farmers but bore liability for payment of claims beyond premium collected. PMFBY is an actuarial model based scheme where token premium is charged and government pays the balance premium quoted by insurance companies selected by states through transparent bidding — full liability of payment of claims is with companies.
Reports suggesting 350% increase in premiums conveniently suppress that government liability was unlimited in the earlier scheme. The 2015-16 type drought, had it happened in 2016-17 or 2017-18 with nearly double sum insured, would have resulted in a huge payout than premium subsidy in PMFBY.
PMFBY has seen a quantum jump in voluntary enrolment of farmers. It has two categories — loanee farmers (those who avail agriculture loan) are compulsorily covered automatically by banks and non-loanee farmers (those who do not take loan) enrol voluntarily. In 2015-16, the year before PMFBY was launched, only 28 lakh farmers opted voluntarily, rising to an additional 1.36 crore farmers in 2016-17. This number stayed constant in 2017-18. Increase in voluntary enrolment, particularly in rain-fed areas, implies its utility as a safety net.
Since launch of PMFBY, India has had two consecutive bumper crop years. Yet, during 2016-17, more than 5.72 crore farmers were insured, with a claim ratio of 75%. And 4.99 crore farmers were insured in 2017-18, with claim ratio of 87% for Kharif 2017. More than Rs 33,000 crore was paid in the first three seasons against farmer premium share of Rs 7,272 crore.
In context of criticism that insurance firms made windfall gains, calamity-hit areas saw high settlements. More than 100% of premium collected in Kerala (210%) and Karnataka (132%) during Kharif 2016, in Tamil Nadu (287%) and Andhra Pradesh (159%) during Rabi 2016-17, and in Chhattisgarh (425%), Odisha (204%), Haryana (201%), and Madhya Pradesh (135%) during Kharif 2017.
During 2017-18, there was a drop in total farmers insured to 4.99 crore from 5.72 crore in 2016-17. This drop is in the compulsory loanee category. Two largest states, Maharashtra and Uttar Pradesh, announced loan waivers, making more than 69 lakh farmers ineligible. Direct benefit transfer with Aadhaar introduced in April 2017 to deliver claims directly in bank accounts erased ghost beneficiaries. This also decreased loanee farmers though voluntary coverage was unaffected.
Technology has speeded up claim settlement. The National Crop Insurance Portal seamlessly links more than 5.5 crore farmers and data entry from more than 1.5 lakh banks and financial institutions is done every season. Government is keen to improve the scheme. Timely claim settlement is the key focus. There are penal provisions on agencies which cause delays — 12% penal interest by insurance companies to farmers for delays beyond 10 days. And 12% penal interest by states to insurance companies if more than three months delay in releasing share of subsidy.
PMFBY has a higher basket of risk coverage — from pre-sowing calamities to post harvest losses — and provides uniform benefits to farmers across India. Insurance is all about spreading the risk. It is unfair to compare claims in relatively good years of 2016-17 and 2017-18 with premium collected, even though this is as high as 80%.
Claims
10% claims fake
The Times of India, Dec 04 2015
Mayur Shetty
1 in 10 insurance claims turns out to be a fraud Insurance claim rauds -which are growing in number and getting more innovative -have put insurers in a dilemma. Companies want to simplify the claims process and wipe out the trust deficit faced by insurers. But this is tough when frauds are close to one in ten claims in some retail categories. “Our estimate is that industry frauds are in the range of 10% of claims, which I feel is a conservative one,“ said Ri esh Kumar, MD & CEO, HDFC Ergo General Insurance. The choice is between being very careful in accepting proposals and liberal in settlement, or in being liberal in accepting proposals and vigilant while sett ing. Excess scrutiny in policy ssuance makes it difficult to sell in a market with low penetration. But delaying claims worsens the trust deficit among individuals, reflected in the belief that getting claims paid is a challenge.
Simplifying claim settlement is something that most companies are trying to do in order to build a retail portfolio.“If a policyholder who has spent lakhs on an overseas trip claims $300 for lost baggage, we would accept the claim,“ said Sanjay Datta, head of underwriting and claims at ICICI Lombard General Insurance.Even state-owned New India Assurance had a few months earlier launched a householder policy that settles claims for breakdown of electronic equipment where all household items would be covered on good faith without the buyer having to declare each individual item or provide proof of ownership.
According to G Srinivasan, chairman, New India Assurance, frauds are expected to be around 10% and the company is trying to address frauds by drawing patterns and through analytics without inconveniencing policyholders.Insurers have also created an electronic database that serves as a blacklist.
The challenge is that fraud patterns are also changing fast.
According to Bhaskar Jyoti Sarma, MD, SBI General, a large chunk of frauds are also in motor insurance.
Claims settlement, 2016: New India the best
New India Assurance tops in claims settlement ratio, Sep 9, 2017: The Times of India

New India Assurance, Royal Sundaram and Universal Sompo have among the highest claims settlement ratios in the nonlife industry. The ratio represents the number of claims settled during a period out of the total claims intimated and is an important indicator of customer service.
According to a report prepared by the Insurance Brokers Association of India (IBAI), the settlement efficiency is not skewed towards any particular segment of the industry . Each of the three segments -public, large private and small private -have leaders and laggards.The IBAI has published a handbook measuring efficiency parameters for non-life companies as of September 2016 to enable customers to take informed decisions while choosing companies.
In the public sector, New India Assurance is miles ahead of its peers with a claims settlement ratio of 71%, while its closest peer United India has a 55.4% ratio. The other two companies -Oriental and National Insuran ce -have ratios of 46.7% and 45.4% respectively .
According to IBAI president Sanjay Kedia, companies with a high component of cashless component in motor and health will have better ratios as their claims are settled immediately after assessment by third-party administrators or affiliated garages.
SC: The situation is alarming/ 2017
Dipak Dash, Curb false insurance claims: SC to govts, January 31, 2017: The Times of India
Holding that instances of fake insurance claims have risen sharply , the Supreme Court has decided to frame guidelines to prevent filing of such “false and fabricated cases“.
Taking serious note of fake insurance claims, the apex court has issued notices to all states and insurance companies to suggest steps to rule out such cases.
Hearing a plea regarding false insurance claims in Ut tar Pradesh earlier this month, the SC expanded the ambit and has sought response from states and other stake-holders to evolve a mechanism to curb such practice.
“The situation is really alarming. Similar scenario cannot be ruled out in other states UTs also, which is required to be looked out,“ a bench of Justice Arun Mish ra and Justice Amitava Roy observed while hearing an appeal filed by Safiq Ahmed against an order passed by the Lucknow bench of Allahabad high court in October 2015.The petitioner's plea for compensation was turned down by the HC as it was also found as a suspected case of fraud.
The HC has set up a special investigation team (SIT) af ter ICICI Lombard, a private insurance firm, had filed a civil revision petition in the court against the fraud played by claimants against it.The company had submitted a list of 64 bogus pending claims filed in different tribunals across districts including in Ghaziabad, Meerut, Lucknow, Moradabad, Gorakhpur, Allahabad, Raibareli and Aligarh.
“The said list suspected fraud cases involved a cumulative claim amount of Rs 8.57 crore approximately . Out of the 64 suspected cases, 29 cases were already adjudicated by the concerned tribunals in favour of the claimants on the basis of police documents and evidence adduced by the claimants,“ a company spokesperson said. The company said one such glaring example was an alleged accident involving a vehicle in May 2012, which was being driven by one Ikrar. However, in a case filed three months earlier, Ikrar was awarded compensation for amputation of his left leg below knee by the Workmen Compensation Commissioner of Ghaziabad, arising out of a road accident. The Allahabad HC in its October 2015 order had referred to the alleged pending bogus claims as “tip of iceberg“.
The HC had observed, “In some cases claims have been filed under Workman Compensation Act as well as under Motor Vehicles Act. Such a loot of public money cannot be allowed to go unchecked and undetected.“
Cannot deny claim on grounds of delayed filing: SC
Nat'l Consumer Panel Directive Set Aside
The Supreme Court has ruled that insurance claims cannot be denied to a person merely on the grounds of delay in filing the claim, holding that “mechanical“ denials on technical bases will cause people to lose confidence in the industry.
A bench of Justice R K Agrawal and Justice S Abdul Nazeer set aside the verdicts of various consumer courts, including the National Consumer Disputes Redressal Commission (NCDRC), which had ruled that insurance companies could deny the benefit of cover for delay in filing the claims. The SC directed Reliance General Insurance Company to pay Rs 8.35 lakh to a Hisar-based customer whose insured truck was stolen but his claim rejected on the grounds of delay in filing it.
“It is true that the owner has to intimate the insurer immediately after the theft of the vehicle. However, this condition should not bar settlement of genuine claims, particularly when the delay in intimation or submission of documents is due to unavoidable circumstances. The decision of the insurer to reject the claim has to be based on valid grounds. Rejection of the claims on purely technical grounds in a mechanical manner will result in loss of confidence of policyholders in the insurance industry ,“ said Justice Nazeer, who wrote the judgment.
The verdict would bring big relief to people who fail to file insurance claims immediately after their vehicles are damaged in accidents or stolen. The court said a practical approach had to be taken in such cases as it was common knowledge that a person who loses their vehicle might not straightaway go to the insurance company, and would first make efforts to trace it.
“If the reason for delay ... is satisfactorily explained, such a claim cannot be rejected on the ground of delay . It is also necessary to state here that it would not be fair and reasona ble to reject genuine claims which had already been verified and found to be correct by the investigator. The condition regarding the delay shall not be a shelter to repudiate the insurance claims which have been otherwise proved to be genuine,“ the bench said.
The court emphasised that the Consumer Protection Act was meant to protect the interest of consumers and the law deserved “liberal construction“. “This laudable object should not be forgotten while considering the claims made under the Act,“ it said.
In the case in question, the vehicle-owner had filed the claim eight days after his truck was stolen as he was busy trying to trace it. The insurance firm rejected his claim, saying he had violated a policy condition that made it mandatory for a policy-holder to inform the firm immediately after any accidental loss or damage to the vehicle.
2016-17: LIC leads
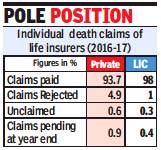
From: January 5, 2018: The Times of India
See graphic:
Individual death claims of life insurers (2016-17)
Can’t deny i claim over driver’s fake licence: SC, 2020
AmitAnand Choudhary, March 5, 2020: The Times of India
The Supreme Court ruled that an insurance company cannot deny claim to the owner of a vehicle involved in a road accident if his driver had falsely claimed to be holding a valid driving licence by producing a fake document.
A bench of Justices Navin Sinha and Krishna Murari said it would not be possible for any owner to make inquiries with regional transport offices all over the country to ascertain the veracity of the driving licence, particularly when he has no reason to doubt its veracity. The SC said wilful breach of the conditions of the insurance policy should be established to deny claim to the insured.
“While hiring a driver, the employer is expected to verify if the driver has a driving licence. If the driver produces a licence which on the face of it looks genuine, the employer is not expected to further investigate into the authenticity of the licence unless there is cause to believe otherwise. If the employer finds the driver to be competent to drive the vehicle and has satisfied himself that the driver has a driving licence there would be no breach of Section 149(2)(a)(ii) and the insurance company would be liable under the policy,” it said. Breach of conditions under Section 149(2)(a) of the Motor Vehicles Act absolves the insurer of its liability to the insured. The section deals with the conditions regarding driving licence. In case the vehicle at the time of accident is driven by a person who is not duly licensed or by a person who has been disqualified from holding or obtaining a driving licence during the period of disqualification, the insurer is not liable for compensation.
The bench said it would not amount to breach of the section when the owner was himself deceived by his driver. “It would be unreasonable to place such a high onus on the insured to make inquiries with RTOs all over the country to ascertain the veracity of the driving licence. However, if the insurance company is able to prove that the owner/insured was aware or had noticed that the licence was fake or invalid and still permitted the person to drive, the insurance company would no longer continue to be liable,” it said.
The apex court set aside order of National Consumer Disputes Redressal Commission which had absolved an insurance company of its liability since no record of the licence of the driver was found with the licensing authority. In this case, the insured vehicle met with an accident with a tractor as a result of which the owner of the vehicle and his daughter died. United India Insurance Company, however, turned down the claim filed by his wife on the ground that the driver did not have a proper driving licence at the time of the accident.
Frauds
2016> 19: Fake motor policies more than double
Mamtha A, July 22, 2019: The Times of India
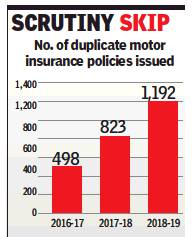
From: Mamtha A, July 22, 2019: The Times of India
Fake motor insurance policies have more than doubled to 1,192 cases from 498 cases, with more than Rs 53 crore worth fake policies sold in India in the last two years, data from IRDAI’s fraud monitoring cell showed.
For the year 2016-17, 498 fake policies were sold, which rose to 823 in 2017-18, the number further increased to 1,192 in 2018-19, finance minister Nirmala Sitharaman told the parliament in a written reply earlier this month. Most of the duplicate policies have been sold to truck and two-wheeler owners, who buy them to avoid scrutiny.
All of these are sold as renewal policies, with almost identical data that is contained in a genuine motor policy, making it difficult to differentiate from the orginal. “A genuine motor insurance policy will cost Rs 10,000, while a fake policy would cost between Rs 5,000-6,000. The vehicle owner is much aware that the fake policy certificate could only help to escape the police, but not help while claiming for damages, however many purchase them,” Sanjiv Dwivedi, head of investigation & loss mitigation team, Bajaj Allianz, said. “About 70% of vehicles in India are not insured.”
“We have filed about 93 cases with the police against fake motor insurance policies in 2018, many of which were sold in Ferozepur in UP, Tiruvananthapuram in Kerala, and Akluj in Maharashtra so far,” Dwivedi added. IRDAI said that it had received complaints directly relating to three entities — AKPCL General Insurance Company in 2016, Gone General Insurance and Marines Technology in 2019 — for fake policy sales, in the past.
Most fake policies have been linked to insuring second hand vehicles, where it is purchased for statutory compliance rather than safety.
“Finding fake policies is nothing new to the insurance sectors. Fake agents mislead customers using our brand name to sell at lower rates,” Sanjay Datta, head of underwriting, claims, reinsurance and actuary of ICICI Lombard, said.
To combat this menace, insurers have started to fix bar codes, which when scanned will throw details of the policy. Some others afix 3D holograms and also educating the police and investigation agencies to differentiate between a original and fake policy.
“Bajaj Allianz has issued a link where the barcode on the policy paper, and help check the authenticity of the policy. We had also conducted training for around 2,580 police officers last year on checking authenticity of the motor insurance policy,” Dwivedi said.
“Besides providing barcode and QR code on the insurance document, 3D hologram stickers were recently introduced to help during police verification,” said SBI General Insurance COO Atul Deshpande.
General Insurance Corporation of India (GIC Re)
The General Insurance Corporation of India (GIC Re) was approved as the ‘‘Indian Reinsurer’’ on 3rd November 2000. As an ‘‘Indian Reinsurer’’ GIC Re has been giving reinsurance support to non-life Insurance companies in India. It continues its role as a reinsurance facilitator by managing Marine Hull Pool, Terrorism Pool and Indian Motor Third Party Insurance Pool on behalf of Indian Insurance industry. The Reinsurance programme of GIC Re aims at optimizing the retention within the country and developing adequate reinsurance capacity.
The Corporation continued to offer maximum support for all classes of business to the Indian insurers. Property and Engineering Risks are covered up to Rs 1500 crore. Whenever there is a requirement to cover a Large Risk beyond Rs 1500 crore, specific Excess of Loss cover is arranged beyond the said limit. The per location capacity of the Terrorism Pool managed by GIC Re has increased to Rs 750 crore with effect from 1.4.2008 from the earlier limit of Rs 600 crore.
Since 1.4.2007, the GIC Re administers the market initiative in respect of Commercial Vehicle Market Third Party Liability policies as a multi-lateral reinsurance arrangement among the participating non-life insurance companies in India. The GIC Re continues to lead the reinsurance programme of the companies in Kenya, Malaysia, Mauritius, Middle-East, Africa and Sri Lanka. In the process, it has emerged as a preferred Reinsurer in the Afro-Asian region. GIC Re is expanding its global presence and now plans to enter the Latin American market having got the 'Eventual Reinsurer' status in Brazil. GIC Re has been selected as the Manager for Nat Cat Pool promoted by the Federation of Afro-Asian Insurers and Reinsurers (FAIR).
During the year 2009-10, the net premium income of the Corporation was Rs 8776.87 crore as against Rs 7402.33 crore in the previous year. The net incurred claims were at Rs 6,856.39 crore, i.e., 84.9 per cent as against Rs 6217.14 crore in the previous year, i.e., 79.6 per cent. Profit after tax was Rs 1774.60 crore as on 31st March 2010 compared to Rs 1407.20 crore as on 31st March 2009. The total assets and networth as on 31st March 2010 was Rs 43842.13 crore and Rs 9133.26 crore, respectively.
The Corporation has its presence in foreign reinsurance business through its Branch offices in Dubai and Londan and a Representative Office in Moscow. A branch office is also being opened shortly in Kuala Lumpur, Malaysia. Apart from reinsurance business, GIC Re continues to participate in the share capital of Kenindia Assurance Company Ltd. Kenya; India International Insurance Pvt Ltd. Singapore; LIC (Mauritius) Offshore Ltd, Mauritius; Asian Reinsurance Corporation. Thailand; East Africa Reinsurance Company Ltd.; Kenya; and Agriculture Insurance Company of India Limited.
Public Sector General Insurers' Companies (GIPSA)
After opening up of the insurance sector and de-linking from GIC in 2000, the four General Insurance Companies, namely, National Insurance Company Ltd., New India Assurance Company Ltd., Oriental Insurance Company Ltd., and United India Insurance Company Ltd., are functioning independently. The four Public Sector General Insurance Companies have a network of 101 Regional Offices, 1395 Divisional Offices, 2880 Branch Offices in India and 55 Overseas Offices.
The gross premium income of the four Public Sector General Insurance Companies during 2008-09 was Rs 19,107 crore as against Rs 17,813 crore during 2007- 08. Profit after Tax for 2008-09 was Rs 508.85 crore as against Rs 2205 crore in 2007-08. The companies have paid a total dividend of Rs141 crore in 2008-09 to the government as against Rs 449 crores in 2007-08.
Disinvestment
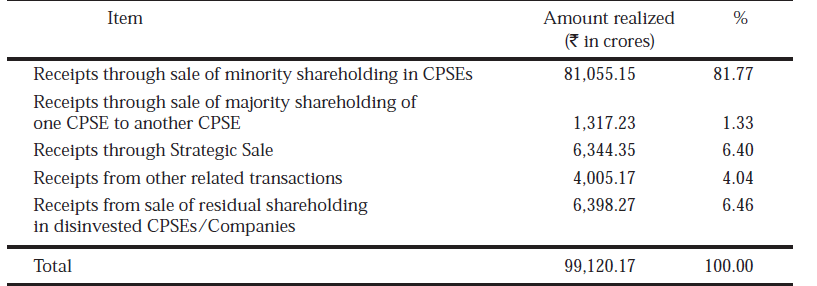
The disinvestment of Government equity in Central Public Sector Enterprises (CPSEs) began in 1991-1992. Since then, it has emerged as a common ground across the polity and as an integral part of Public Finances in India's economic growth story. The year-wise resources mobilized through disinvestment are given in the Table. From 1999-2000 till 2003-04, the emphasis of disinvestment changed in favour of Strategic Sale viz., sale of large block of shares along with transfer of management control to a Strategic Partner identified through a process of competitive bidding. After 2004-2005, disinvestment realizations have been through sale of small portions of equity. The total proceeds from disinvestment between 1991-1992 and 31st March, 2011 amounted to Rs. 99,120.17 crore, consisting of the following:
Item Amount realized %
(Rs. in crores)
Receipts through sale of minority shareholding in CPSEs 81,055.15 81.77
Receipts through sale of majority shareholding of one CPSE to another CPSE 1,317.23 1.33
Receipts through Strategic Sale 6,344.35 6.40
Receipts from other related transactions 4,005.17 4.04
Receipts from sale of residual shareholding in disinvested CPSEs/Companies 6,398.27 6.46
Total 99,120.17 100.00
Policy Framework
I. One of the main objectives of the disinvestment policy is to develop people's ownership of Central Public Sector Enterprises so as to let them directly share in the wealth and prosperity accruing to the country's economy through the combined enterprise of the business ventures in the Public Sector. The policy inter alia ensures that Government equity does not fall below 51% and Government retains management control.
II. The Government, on 5th November 2009 approved an action plan for disinvesting Government equity in profit making CPSEs.
III. Approach for disinvestment
(i) Already listed profitable Central Public Sector Enterprises (CPSEs) not meeting the mandatory public shareholding of 10% are to be made compliant by public offering out of Government shareholding or issues of fresh equity by the CPSEs concerned or a combination of both;
(ii) All unlisted CPSUs having positive net worth, no accumulated losses and having earned net profit for three preceding consecutive years, are to be listed through public offerings out of Government shareholding or issue of fresh equity by the company or a combination of both; and
(iii) Further public offerings by listed CPSEs taking into consideration their capital investment requirements with GoI simultaneously or independenty offering a portion of its shareholding in such CPSEs;
(iv) All cases of disinvestment are to be decided on a case by case basis as each CPSE has different equity structure, financial strength, fund requirement, sector of operation, etc., factors that will not permit a uniform pattern;
(v) Government retains at lease 51 per cent equity and management control in all cases of disinvestment through public offerings.
Constitution of National Investment Fund
The Government has constituted a "National Investment Fund" (NIF) in 2005-06, into which the proceeds from disinvestment of Government equity in CPSEs would flow in. NIF is maintained outside the Consolidated Fund of India and is professionally manged to provide sustainable returns without depleting the corpus. Of the annual income of the Fund, 75% is envisaged to be used to finance selected social sector schemes, which promote education, health and employment.
The residual 25% of the annual income of the Fund is envisaged to be used to meet the capital investment requirements of profitable and revivable CPSEs that yield adequate returns, in order to enlarge their capital base to finance expansion/ diversification. The corpus of the Fund as on 31st March, 2010 is Rs. 1814.45 crore. In view of difficult economic situation, the disinvestment proceeds channelised into NIF from April 2009 to March 2012 (three years) would be used in full to support specific social sector schemes identified by Planning Commission/Department of Expenditure. Status quo ante of NIF will thus get restored after three years, i.e., after April 2012.
Use of Disinvestment Proceeds
From April 2009, the disinvestment proceeds are being used for funding the capital expenditure under the social sector schemes of the Government, namely:-
(i) Mahatma Gandhi National Rural Employment Guarantee Scheme;
(ii) Indira Awas Yojana;
(iii) Rajiv Gandhi Gramin Vidyutikaran Yojana;
(iv) Jawaharlal Nehru National Urban Renewal Mission;
(v) Accelerated Irrigation Benefits Programme;
(vi) Accelerated Power Development Reform Programme.
During 2004-05, Government realized t 2,684.07 crore from the sale of 43.29 crore equity share of t 10 each of National Thermal Power Corporation Ltd., t 64.81 crore from the sale of shares to employees of IPCL and t15.99 crore as balance amount of realization from the Offer for Sale in ONGC.
During the year 2005-06, the Government realized a sum of t1,567.60 crore from the sale of 8 per cent of equity, out of its shareholding of 18.28 per cent, in Maruti Udog Limited (MUL), to public sector financial institutions and banks. The average realization was t 678.24 per share. Further, t 2.08 crore were received by the Government, from the sale of 31,507 equity shares in MUL to officers/employees of MUL at a price of t 660 per share.
During the year 2007-08, the Government realized a sum of t4,181.39 crore from the sale of 10.27 per cent equity of Maruti Udyog Limited (MUL); and 10% paid up equity each of Power Grid Corporation of India Ltd. and Rural Electrification Corporation India Ltd.
During the year 2009-10, the Government realized an amount of t23,552.93 crore from sale of 5 per cent equity in NHPC Ltd., 10 percent in Oil India Ltd., 5 per cent in NTPC Ltd., 5 per cent in REC Ltd. and 8.38 per cent in NMDC Ltd. During the year 2010-11, the Government realized an amount of t22,144.21 crore from sale of 10.03 per cent in SJVN Ltd., 10 per cent equity each in Engineers India Ltd., Coal India Ltd., Power Grid Corporation of India Ltd., MOIL Ltd., and Shipping Corporation of India Ltd.
Rank in the world, 2017
India's national reinsurer General Insurance Corporation (GIC Re) has moved up two places in world reinsurance rankings following the implementation of the government's new crop cover scheme. With premium income growing 87% in FY17, the corporation has been driving reinsurance growth in Asia despite China slowing down.
According to AM Best, a ratings agency which specialises in the insurance industry , GIC Re is now the twelfth-largest reinsurer in the world, up from 14th position in 2016 The corporation has overtaken two companies -US-based Transatlantic and Bermuda-headquartered Everest Re. To break into the global top 10, GIC will need to outgrow Partner Re and Korean Re, which are ranked 11 and 10 this year. These two companies have a top line that is 2.8% and 6.6% more than that of GIC Re.
Reinsurance companies take on the risks from insurance companies. Insurers share their business with reinsurers to reduce pressure on their capital and to hedge against extreme losses.
The Indian market saw quadrupling of agricultural insurance premium. This -together with growth in other segments such as motor and health, and market expansion in general apart from continued focus on geographical diversification through growth in international book -led to a robust 82% higher premium for GIC Re. This contributed to the improvement in ranking.
While India is a highgrowth market, GIC Re does face some challenges this year. According to the latest AM Best report, GIC is likely to continue to grow over the short term, though at a slower pace. This is because more foreign reinsurers have set shop.
Judgements, judicial
2020: Policy not activated but money paid: cover will be available
An insurance company can’t deny compensation because a policy was not activated even 15 days after the client had paid the premium, the apex consumer commission, NCDRC, has ruled. Norms of insurance regulator IRDAI say the policy has to be issued or rejected within 15 days from the date of full payment of premium by a client.
Taking up a revision petition filed by Reliance Life Insurance Company Ltd challenging the decision of the Madhya Pradesh State Consumer Commission, a single NCDRC bench comprising member Dinesh Singh not only upheld the Rs 4.8 lakh compensation awarded by the state entity, but imposed a penalty of Rs 50,000 on the firm. It ordered the firm to pay another Rs 50,000 to the complainant as cost of litigation.In this case, MP’s Radhyeshyam Mourya, had taken “Reliance Super Automatic Investment Plan Policy” on May 5, 2009 with assured sum at Rs 4.8 lakh and had paid annual premium of Rs 20,000. He died in a road accident on May 27. But the policy was issued two days after his death.
Policy valid till cancellation notice of insurer: HC
April 5, 2025: The Times of India
A vehicle continues to be insured until the policyholder receives a formal cancellation notice, Karnataka HC held in arecent judgment, asking an insurer to pay over Rs 1.2 lakh as it could not prove that a customer had received formal intimation about annulment of coverage. P Yadava Rao’s car was damaged after being hit by a lorry in July 2007. He moved a motor accident claims tribunal seeking compensation. The insurance company was exonerated on the grounds that it had cancelled the policy as the cheque issued for payment of premium was dishonoured.
Court held that it was the insurer’s responsibility to inform vehicle owner about policy cancellation, stressing there must be proof of addressee having received intimation. TNN
Maternity benefits
Applicable to living, dead childbirths
A private insurance company’s contention that maternity benefits are applicable only to live births came under criticism recently from a Bengaluru consumer court. The judges slammed the firm’s decision to deny a Bengaluru techie her policy claim after medical termination of her 23-week-old twin foetuses.
After a nearly five-year battle by the woman, the court ordered full payment as well as compensation. Judges of the consumer forum stated that childbirth doesn’t indicate living or dead child. It is a settled proposition of law that a child in its mother’s womb is entitled to all rights.
2016: ICICI Lombard becomes no.4
Mayur Shetty, Aug 06 2016/ For first time, pvt general insurer breaks into top 4 Private sector nonlife insurer ICICI Lombard has overtaken state-owned Oriental Insurance to become the third-largest in terms of gross written premium. This is the first time after the industry opened up in 2000 that a private insurer has surpassed a PSU counterpart.
ICICI Lombard ended the quarter-ended June 2016 with gross premium of Rs 2,880 crore. This has given the private insurer a lead over Oriental Insurance, which recorded premium income of Rs 2,508 crore after a 15% growth with a 9% market share.
The first quarter has been good for non-life companies, which collectively grew nearly 17%. Private insurers grew at a much faster rate (about 21%) as against public sector companies (nearly 14%). For one and half decades, the top four slots have been consistently held by New India Assurance, which continues to be the market leader, and three other public sector units -National Insurance, Oriental Insurance and United India Insurance. PSU insurers continue to have a market share of nearly 52%. However, there appears to be some consolidation in business among private compani es with the top five companies ICICI Lombard, Bajaj Allianz (6% marketshare), IFFCO Tokio (4%), Tata AIG (3.4%) and Reliance General (3.2%) accounting for more than half the business for private insurers.
2016-19
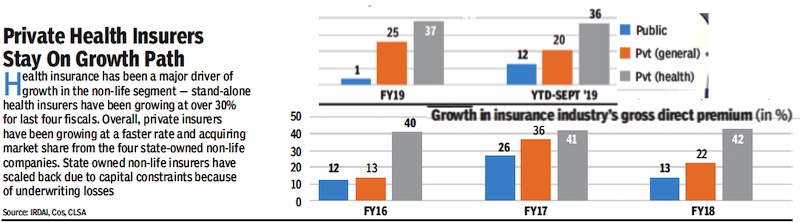
From: December 4, 2019: The Times of India
See graphic:
Growth in insurance industry's gross direct premium (in %), FY16- FY20
2017: Oriental reclaims No.4 rank
Private insurer ICICI Lombard lost its edge over public-sector insurer Oriental this March as it saw its market share dip to 8.43%. For a short span of nearly a year, ICICI Lombard managed to enter the top 4 slot among general insurers -a bracket exclusively held for more than 15 years by New India Assurance, National Insurance, Oriental Insurance and United India Insurance.
But Oriental Insurance has regained lost territory and moved ahead of the private player with a market share of 8.46% for the month of March, according to the Insurance Regulatory and Development Au thority of India (IRDAI) data.
Last August, ICICI Lombard overtook Oriental Insurance to become the fourth-largest insurer (market share 11%) with gross written premium of `2,880 crore, 41% y-o-y increase.The milestone was significant as the it was the first time a pri vate insurer had beaten a public-sector player since the industry opened in 2000. As of March 2017, ICICI Lombard had written `10,725 crore in gross direct premium, compared to Oriental Insurance's `10,792 crore.ICICI Lombard's growth rate was 32.56% for the month of March vs Oriental's year-overyear growth of 29.79%.
2017, July: private insurers beat PSUs
Rachel Chitra, In a 1st, pvt non-life insurers beat PSUs, August 11, 2017: The Times of India
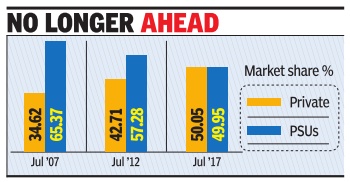
For the first time since the market opened up in 2000, private non-life insurance companies have raced ahead of public sector giants. As of July 2017, private insurers had 50.05% of the market share versus 49.95% for their state-owned rivals. Of the total premium income of Rs 43,077 crore generated by the industry up to July , private companies have garnered Rs 21,561 crore while PSUs have booked Rs 21,515 crore.
Private companies have grown at 26% while public sector giants have increased their premium income by12%. The slower growth by PSU companies appears to be a deliberate strategy as they focus on margins more than top line ahead of their public offerings. Among the four governmentowned companies, New India Assurance and National Insurance have announced their intent to go public and Chennai-based United India has said that it will go slow on motor and health to improve underwriting margins.
What appears to have tipped the scales this year is crop insurance, said Sujay Banerji of Ori ental Insurance Company .“Public sector giants have not had any major crop insurance business so far. Private sector leaders like ICICI Lombard have booked significant growth in this space. With crop insurance emerging as the third-major line of business for the Indian insurance industry , this has definitely created a wedge for PSUs,“ said Banerji. TOI reported in April that the crop insurance industry has been a driving factor for the industry , posting 32% growth and crossing the Rs 1-lakh-crore mark for the first time. Tapan Singhel, CEO, Bajaj Allianz General Insurance, said, “Private insurers have always been in the crop insurance business, but this gained particular momentum after the launch of the Pradhan Mantri Fasal Bima Yojana (PMFBY) last year.“
Another reason for the loss in marketshare is the change in strategy PSUs have adopted.New India CMD G Srinivasan has said that in a bid for quality over quantity , the insurer has increased premium rates.Growth rates of the PSUs (average 11.97%) continue to remain muted in comparison to the private industry (26.25%).
PART B
Types of insurance schemes
Losses, sector-wise, 2019-21
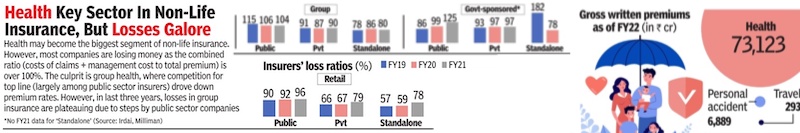
From: Dec 15, 2022: The Times of India
See graphic:
Sector-wise losses in non-life insurance, 2019-21
Accidents
Mosquito bite an accident
In what could be a path-breaking order, the National Consumer Disputes Redressal Commission has held that a malaria death caused by mosquito bite is an accident, and directed the insurer to honour its policy to a widow.
“An accident is something that happens unexpectedly and is not planned, said the commission. “It can hardly be disputed that a mosquito bite is something which no one expects and which happens all of a sudden without any act of omission on part of the victim,“ said Justice V K Jain, presiding member of NCDRC.
The order came on a claim filed by Mousumi Bhattacharjee, who lost her husband in November 2012 to malaria in Mozambique where he worked in a tea factory . The husband, Debasish, a Kolkata resident, had availed of a policy of the National Insurance Company called “Bank of Baroda Home Loan Suraksha Bima“ to cover death by accidents. He paid a one-time premium for the sum insured, Rs 13.15 lakh, to be paid in case of “death due to accident“. But when his widow filed a claim, the insurance com pany rejected it saying a mosquito bite was not an accident under the policy , and that malaria was a disease. But all three consumer fora, right from the district and state consumer forums to the apex National Consumer Commission, held the company's stand incorrect.
The national commission observed that the insurer had included snake bites, dog bites and frost bites under the `accident' category . The commission also cited Black's Law dictionary that describes an accident as “an unanticipated and untoward event that causes harm“. Consumer activist Jehangir Gai said the judgment would benefit several policy holders, especially those who are victims of dengue and malaria as the same interpretation will apply to dengue also.“
While welcoming the decision, another veteran consumer activist Shirish Deshpande, however sounded a note of caution. “The commission has equated dog and snake bites with mosquito bites. But malaria is endemic in nature. The judgment may need to be tested finally by the SC as it may open floodgates for such claims.“
Murder covered by Accident Policy: Court
A Delhi district consumer forum has trashed an insurance company’s reason for rejecting a claim by the kin of a man who was allegedly murdered. The forum said that delay in filing the claim and the fact that the man was murdered cannot be grounds to deny an insurance claim.
The insurance company was accordingly directed to pay Rs 5 lakh, along with 9% interest, to the mother of the deceased, besides an extra Rs 25,000 for causing “mental agony and pain”.
“Insurance company has failed to place on record any documentary evidence to prove that murder is out of the purview of the personal accident policy,” observed the forum bench. It relied on a circular of the Insurance Regulatory and Development Authority, which says that rejection of a claim should be based on sound logic and valid grounds and no genuine claim should be rejected merely because there was a delay in lodging the claim. New India Assurance Co. Ltd had argued that the deceased was murdered in a “planned manner” and, therefore, the case was out of the purview of the accident policy.
The forum had to deal with the question whether the insurance company could rely on the terms and conditions that were never supplied to the insured. “The answer is in the negative,” the forum said. It, therefore, held that unless terms and conditions are supplied to the complainant prior to the policy, its clauses cannot be enforced.
Munish Kumar died on May 30, 2012, following which his parents approached his bank to lodge a claim against his personal accident insurance policy. Bank officials, however, said it had not issued the policy, but the insurance company had. It claimed only to be a facilitator.
In May 2013, the insurance company repudiated the claim on the ground that there was an inordinate delay of 159 days in the submission of the claim papers from the day of Kumar’s death.
Appearing for the mother, advocate Sahil Mongia told the forum that his client had sent a representation to the insurance company on December 5, 2013 but nothing came of it. Thereafter, notices were sent to the bank and the insurance company but no one appeared for the former.
The insurance company contested the claims of the mother citing the 159 day delay. It also argued that the complainant ought to have informed it about the death of her son. But the forum pointed out that the company had not filed any evidence, which could be considered. “On the contrary, the claim should be dealt on merit,” it said.
Car/ motor vehicle insurance
Delay in notifying insurer about theft no ground to deny claim: SC
January 25, 2020: The Times of India
Delay in notifying insurer about car theft no ground to deny claim: SC
NEW DELHI: The Supreme Court said mere delay in intimating the insurance company about theft of a vehicle should not be a ground to deny insurance claim if the aggrieved person had informed police on time.
A bench of Justices N V Ramana, R Subhash Reddy and B R Gavai agreed with the SC's verdict of 2017 in which it had held that it would be taking a hyper technical view if the claimant is denied claim on the ground that there is some delay in intimating the insurance company about the theft. The insurance company, however, claimed it is stipulated in the Standard Form for Commercial Vehicles Package Policy that claimant will immediately inform the company in case of theft and claim can be denied in case of not complying with the condition.
Rejecting the plea of the company, the bench said, "...if police is immediately informed about the theft, the police machinery can be set in motion and steps for recovery of the vehicle could be expedited. In a case of theft, the insurance company or a surveyor would have a limited role...We, therefore, hold that when an insured has lodged an FIR immediately after the theft..., mere delay in intimating the insurance company... cannot be a ground to deny the claim of the insured”.
No relief if owner negligent
The Times of India, Nov 14 2015
Sana Shakil
No relief if vehicle lost due to owner's fault
The owner of a vehicle cannot claim any compensation from an insurance company in case his vehicle is damaged or stolen due to his own negligence, a trial court said.
The court made the observation while denying an insurance claim to Jamun Pandey , whose truck was stolen after his driver Ram Nandan forgot the keys in the vehicle and left it unattended for some time in an unauthorised area. “The insured vehicle was stolen due to the negligence of the driver of the plaintiff. The plaintiff is guilty of breach of terms and conditions of the insurance policy . I, hereby, hold that the plaintiff is not entitled to any relief of recovery from the defendant as asked for in the plaint,“ additional district judge Kamini Lau said.
The court was hearing a suit filed by Pandey , who had claimed Rs 6.2 lakh from SBI General Insurance Company . The insurance policy was valid from December 14, 2012-December 13, 2013, and Pandey's truck went missing on October 25, 2013, from a spot near Pratap Nagar Metro station. Pandey , in his plaint, said he was entitled to get the insurance amount according to the company's policy . However, the company strongly opposed the plea, saying that Pandey was guilty of gross negli gence that led to the theft. The court agreed with the defendant's submission and pointed out several discrepancies in Pandey's plaint.
“...Therefore, in view of these four different versions regarding the details of the theft, it is clear that Pandey and Nandan are only trying to cover up their negligence in safeguarding the insured vehicle against loss or damage,“ the court said.
Discussing the facts of the case, the judge said, “The sta tement that one key had gone with the vehicle clearly establishes that Ram Nandan had left it in the vehicle, while leaving the truck unattended for at least one hour fifteen minutes as per his own admission.But from the record of the FIR, the time appears to be much longer since the information of the theft was given to police in writing at 8.30am on October 25, 2013, in spite of the distance of the police station from the place of theft being merely a kilometer away“.
…but unlocked car no grounds to reject theft claim
A consumer forum has ruled against an insurance company that rejected a car theft claim on the grounds that the driver left the vehicle unlocked while visiting a washroom for a few minutes. The forum has ordered the insurance company to pay Rs 5.22 lakh, along with a compensation of Rs 40,000, to the owner of a Skoda car stolen from a heavily secured and guarded Marine Lines building in 2012.
The complaint was submitted before the Central Mumbai District Consumer Disputes Redressal Forum in 2015 by the owner of the car, Ms Banswara Syntex Limited, against TATA AIG Gene ral Insurance Co Ltd. The complaint said that, on May 7, 2012 the car was parked at a parking slot of the company's director.
The driver of the car slept in the vehicle for the night.The following morning, after the driver returned from a trip to the washroom, he found that the car was not in the parking spot.
A complaint was lodged with police and on May 9, 2012, the RTO was informed. The insurance company was intimated and the claim submitted. However, the insurance company repudiated the claim through a letter dated March 25, 2013 on the grounds that proper care was not taken, and the vehicle was left unattended without locking it. It said that this was a breach of the policy conditions.
The complainant said that the claim was repudiated on the basis of the insu rance company investigator's report. The advocate pointed out that the report said, “It was found that the location is well secured and guarded by a fleet of security persons“. He further submitted that the investigator report was binding on the insurance company . The forum said that it was a well-settled law that the insurance company could not avoid the report submitted by investigator without proper reason.
While pointing to the investigator's report, the forum said, “Merely because the vehicle was not locked, it cannot be said that it was left unattended. In the instant complaint before us, the vehicle was parked at the parking place under security .The opponent has wrongly repudiated the claim.“
Overloading no reason to deny claim: SC
The Times of India Jan 10 2016
AmitAnand Choudhary
Overloading of a vehicle cannot be the sole ground for an insurance company to reject claims for damages caused to the vehicle in a road accident, the Supreme Court has ruled while quashing National Consumer Disputes Redressal Commission's order that loss caused to overloaded vehicle won't be compensated.
A bench of Chief Justice T S Thakur and justice V Gopala Gowda held that carrying more passengers than the permitted capacity in an insured vehicle does not amount to a fundamental breach of the terms and conditions of the policy.
It said the insurance com pany had to prove that the accident was caused because of the overloading to escape the liability of paying claims.The bench directed the insurance company to reimburse claim to the damages caused to a goods-carrying vehicle travelling with five passengers while its seating capacity was only two, including the driver.
The bench said the insur ance company could deny claims only in cases where breach of insurance policy was so fundamental in nature that it brought the contract to an end. “The insurance company , in order to avoid liability must not only establish the defence claimed in the proceeding concerned, but also establish breach on the part of the ownerinsured of the vehicle for which the burden of proof would rest with the insurance company ,“ it said.
The bench quashed the order passed by NCDRC and Haryana State Consumer Disputes Redressal Commission which had allowed plea of insurance company that overloading could be a ground for denying claim for the damages.
48-hour limitation on intimation of theft
If your car is stolen, there’s no time bar to claim insurance
Rebecca Samervel, TNN | Jun 10, 2013
MUMBAI: A consumer forum has held that the condition with regard to the time limit in intimating an insurance claim is not mandatory but directory. The forum directed Oriental Insurance Company to pay Rs 1.54 lakh compensation along with the insured amount of Rs 4.86 lakh to a Mulund-based man whose vehicle was stolen. The company had repudiated his claim on the ground that he had not intimated them about the claim within the mandatory 48-hour period.
The forum cited a state commission order which said, "This clause is meant for the interest of the insured, in order to facilitate the scrutiny of the claim. This clause therefore, cannot be used in determent to the interest of the insurer."
The vehicle owner Chetan Kohli said that he purchased the Bolero Sport 7 star vehicle for Rs 4.86 lakh on December 18, 2009. He alleged that on the morning of January 8, 2010, he could not find his vehicle at the space in which it was parked and eventually realised that it was stolen.
Kohli immediately informed the police and an FIR was lodged. He also informed the insurance company about the theft and told them that he wanted to file the claim. The company, however, asked Kohli to visit its office along with all the documents of the vehicle. He in turn informed them that since the vehicle was new he did not have the papers and had to collect them from the RTO Office.
The company advised Kohli to first collect the vehicle papers and RTO registration papers and then file the claim form. However, when he finally managed to procure the documents and submit the claim in March 2010, his claim was rejected on the ground that it was not intimated within the mandatory period of 48 hours.
Aggrieved, Kohli filed a complaint on August 18, 2010 in the South Mumbai District Consumer Disputes Redressal Forum. He alleged that the insurance company never informed him that there was a mandatory submission time. Kohli said that he was wrongly advised to get the papers first and then contact the insurance company. In the forum, the insurance company iterated its stand.
The forum said that Kohli had specifically informed the company that he did not have the documents, immediately after the theft of his vehicle occurred. It held that under such facts and circumstances the repudiation was not justifiable. "We therefore, hold that the opposite party (insurance company) cannot repudiate the genuine claim of the insured simply on the ground that there was no communication within the stipulated point of time," the forum said.
2015-16: number of uninsured vehicles (60% two-wheelers)
Somit Sen, 60% of vehicles on Indian roads don't have insurance, Jan 24, 2017: The Times of India
Over 5 Lakh Accidents In 2015 Killed 1.5 Lakh People
Nearly 60% of the vehicles plying on Indian roads are uninsured, most of them motorcycles and scooters. The data has been complied by General Insurance Council (GIC), which represents the country's general insurers.
In 2015-16, India had around 19 crore registered vehicles; of these, only 8.26 crore were insured, said GIC secretary general R Chandrasekaran. The situation was similar in 2012-13, when the total number of vehicles, including two-wheelers, cars and heavy vehicles, registered in the country stood at 15 crore, of which only 6.02 crore were insured. The figures are alarming since India's roads are notorious for their high accident rate, with 2015 alone recording over 5 lakh road crashes. Two-wheelers were in volved in 29% of the accidents in 2015, cars and jeeps in 23%, and buses in 8.3%.
Transport experts point out the need for every vehicle to be insured as those without an insurance cause “huge liability to mishap victims“.
2016: Number of uninsured vehicles (40%: four-wheelers)
The Times of India, August 11, 2016
Dipak Dash
40% of cars have no insurance
Nearly 60%of two-wheelers and 40% of four-wheelers plying on Indian roads have no insurance cover, insurance industry majors have informed the road transport ministry.
Besides being in violation of regulatory norms, such vehicles also pose a risk to other road users as anyone hit by such a vehicle has little chance of getting compensation.
Insurance firms have supported the ministry's proposal to impose a hefty fine of Rs 2,000 to Rs 4,000 for non-compliance with the mandatory provision of third party insurance. TOI has learnt that both private and public insurance firms have backed the provision of capping compensation for road crash victims at Rs 10 lakh.
“They have shared how the average com pensation for fatal crashes is about Rs 6 lakh in nearly 80% cases and that too such payment is made after 4-5 years. In the amendments proposed in the Motor Vehicles Act, we have provisioned for making the payment within 30 days.
However, people will have the option to seek higher compensation by taking the matter to claims tribunal,“ said a ministry official.
Premium on third-party insurance/ 2017
Udit Mukherji, IRDAI offers relief to large car owners, Mar 30, 2017: The Times of India
In a minor relief to owners of large cars, the insurance regulator has rolled back part of the hike in premium on the mandatory motor thirdparty insurance.
As against the 50% hike in rates proposed earlier, the Insurance Regulatory and Development Authority of India (IRDAI) has notified new rates at 40% from April 1.
On small cars (sub-1,000cc), the regulator has stuck to its earlier proposal of not revising rates, which will continue at Rs 2,055 in FY18. This is the first time since 2013 that small cars have been spared from any hike in third party motor insurance premium.
In its final order on Tues day , IRDAI has not proposed hike in third party rates for cars like Alto 800, Santro, Eon, Kwid, Wagon R, Estillo and Celerio. This category constitutes over 30% of the car sales in India and more than 50% of the total private vehicles in the country .
In the 1,000-1,500cc category, the premium has been hiked by 40% from Rs 2,237 to Rs 3,132.The category of vehicles over 1,500cc will also face a similar hike to Rs 8,630 from Rs 6,164.
However , general insurers opined that the possibility of reaching break-even in the third party insurance business would be bleak following the non-revision of rates in the sub-1,000cc category .
The loss ratio (ratio of cla ims to premium income) in the regulated third party insurance business is more than 130%, which implies that for every Rs 100 income, expenses is Rs 130.The third party insurance premium for small cars was Rs1,229 when the new mechanism started. Since then there has been an increase of over Rs 830 in four years, or 67.5%.
PUC must for renewal of vehicle insurance: SC/ 2017
HIGHLIGHTS
• Supreme Court wants owners to produce PUC certificates if they want their vehicle's insurance renewed
• The court also asked the Centre to ensure that all petrol pumps have PUC centres
• The court granted 4 weeks to the Centre to ensure that there are functional PUC centres in NCR
NEW DELHI: In a bid to curb pollution, the Supreme Court issued a directive that insurance of a vehicle will not be renewed unless the owner provides pollution under control (PUC) certificate.
Among the other slew of directions, the bench headed by Justice Madan B Lokur also asked the Ministry of Road Transport and Highways to ensure that all fuel refilling centres in the National Capital Region (NCR) have PUC centres.
The apex court granted four weeks time to the Centre to ensure that there are functional PUC centres in NCR to ensure that vehicles plying have PUC certificate. The court considered the suggestions given by Environment Pollution Control Authority (EPCA). The bench was hearing a PIL filed by environmentalist M C Mehta way back in 1985 dealing with various aspects of pollution.
3-year 3rd-party cover must for new cars: SC
July 21, 2018: The Times of India
From September 1, 2018, people buying new four and two-wheel vehicles will have to cough up three and five years’ premium, respectively, for third-party insurance upfront.
The Supreme Court ordered that no new vehicle will be sold without the mandatory third-party insurance cover for the prescribed period.
Currently, vehicle owners are required to buy oneyear third-party insurance cover and they need to renew it annually. It’s an offence to ply any vehicle without valid third-party insurance. Since the SC order is only on third-party insurance, owners will have the option of renewing the comprehensive insurance cover annually.
Of 18cr registered vehicles, only 6cr insured: Amicus
The insurance industry may come up with similar three and five years’ comprehensive policy in future for the convenience of vehicle owners. A bench of Justices Madan B Lokur and Deepak Gupta accepted the recommendations of the SC-appointed committee on road safety for mandatory insurance cover for the extended period as most vehicle owners do not renew their insurance cover after the first year, leaving road accident victims vulnerable as they are deprived of compensation.
TOI had first reported on April 2 about the committee’s recommendations to insurance regulator IRDA to introduce such policies. The recommendation was made considering the submission of IRDA that a majority of twowheeler owners don’t renew their insurance cover after the first year and about 60% of such vehicles on the roads don’t have insurance.
Advocate Gaurav Agrawal, who is assisting the court as amicus curiae, told the bench that only 6 crore of the 18 crore registered vehicles are insured. Accepting his plea, the bench directed IRDA to take steps to comply with the order. IRDA said it was ready to provide third-party insurance for the extended period but pleaded the court not to make it mandatory. The bench, however, rejected its contention and asked it to take the necessary steps to implement its order.
Auto companies’ control of insurance distribution
Mayur Shetty, January 11, 2020: The Times of India
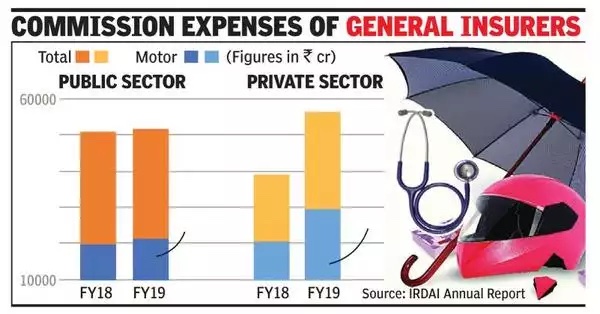
From: Mayur Shetty, January 11, 2020: The Times of India
MUMBAI: The dynamics of motor insurance in India is set to change with the insurance regulator taking a tough stance on auto companies controlling insurance distribution through broking firms.
In December 2019 and January 2020, the Insurance Regulatory and Development Authority of India (IRDAI) penalised a host of insurance broking firms, including Maruti Insurance Brokers, Hero Insurance Broking and Toyota Tsusho Insurance Broking — all linked to auto manufacturers. The fines ranged from Rs 1 crore to Rs 3 crore. The regulator also fined brokers like SMC and Aditya Birla Insurance Brokers for their dealing with auto companies.
Insurance company officials say that fining brokers for dealing with select companies could now open up the business for two dozen companies. Customers could benefit if upstart companies start quoting low rates to get a toehold in the motor business.
In all the cases, the charge was that customers who bought new cars were being denied choice and were indirectly forced to buy from a handful of insurance companies that were empanelled with the broking firms. Another point raised by the regulator was that all the companies in the panel were offering the same rates, indicating that there was some kind of price-fixing. Third, the regulator has identified cases where insurance companies have paid more than the permissible premium by reimbursing costs
It is an open secret in the insurance industry that auto dealers control motor insurance distribution. While the customer is given a choice of companies, they are the ones which are on the panel and often the pricing is similar. The customer is free to buy the insurance from any company, but the dealer — by quoting a blended price — leads the customer to believe that he is willing to bear the insurance cost.
The court order making it mandatory for car buyers to take out a three-year cover and two-wheelers a five-year cover has put more power in the hands of the dealer.
Although the insurance distribution firms are owned by auto companies (described as OEMs, or original equipment manufacturers by the regulator), most of the earnings are passed on to dealers.
Given that the motor insurance market in India stood at over Rs 64,000 crore, the commission runs into several thousand crore (see graphic). They are a major source of revenue for the auto dealers who have to deal with thinning margins on auto sales. Besides the earning from selling insurance, dealers benefit as insured cars come back to them for cashless claims servicing and provide their workshops with assured business.
Auto companies’ control of insurance distribution
Mayur Shetty, January 11, 2020: The Times of India

From: Mayur Shetty, January 11, 2020: The Times of India
MUMBAI: The dynamics of motor insurance in India is set to change with the insurance regulator taking a tough stance on auto companies controlling insurance distribution through broking firms. In December 2019 and January 2020, the Insurance Regulatory and Development Authority of India (IRDAI) penalised a host of insurance broking firms, including Maruti Insurance Brokers, Hero Insurance Broking and Toyota Tsusho Insurance Broking — all linked to auto manufacturers. The fines ranged from Rs 1 crore to Rs 3 crore. The regulator also fined brokers like SMC and Aditya Birla Insurance Brokers for their dealing with auto companies.
Insurance company officials say that fining brokers for dealing with select companies could now open up the business for two dozen companies. Customers could benefit if upstart companies start quoting low rates to get a toehold in the motor business.
In all the cases, the charge was that customers who bought new cars were being denied choice and were indirectly forced to buy from a handful of insurance companies that were empanelled with the broking firms. Another point raised by the regulator was that all the companies in the panel were offering the same rates, indicating that there was some kind of price-fixing. Third, the regulator has identified cases where insurance companies have paid more than the permissible premium by reimbursing costs
It is an open secret in the insurance industry that auto dealers control motor insurance distribution. While the customer is given a choice of companies, they are the ones which are on the panel and often the pricing is similar. The customer is free to buy the insurance from any company, but the dealer — by quoting a blended price — leads the customer to believe that he is willing to bear the insurance cost.
The court order making it mandatory for car buyers to take out a three-year cover and two-wheelers a five-year cover has put more power in the hands of the dealer.
Although the insurance distribution firms are owned by auto companies (described as OEMs, or original equipment manufacturers by the regulator), most of the earnings are passed on to dealers.
Given that the motor insurance market in India stood at over Rs 64,000 crore, the commission runs into several thousand crore (see graphic). They are a major source of revenue for the auto dealers who have to deal with thinning margins on auto sales. Besides the earning from selling insurance, dealers benefit as insured cars come back to them for cashless claims servicing and provide their workshops with assured business.
Cinema
2017: Bahubali 2: The Conclusion (2017) , Enthiran 2…
Future Generali covers Bahubali 2 for Rs 200cr, May 5, 2017: The Times of India
Indian Movie Industry Boosts Insurance Biz
The movie Bahubali 2: The Conclusion, which has set cash registers ringing at the box office, has been good for insurers as well. The big-budget movie was insured for over Rs 200 crore by Future Generali, and the cover has concluded without any major claim.
The Rs 250-crore movie -an epic historical fiction, directed by S S Rajamouli and produced by Shobu Yarlagadda and Prasad Devineni -has involved major investments in elaborate sets and is touted to be the most expensive film in India till date. There are reports that the yet-to-release Rajnikanth's Enthiran 2 (Robot), which has a budget of Rs 450 crore, is insured for Rs 300 crore by stateowned insurers, which makes it the largest film cover.
Krishnamoorthy Rao, MD & CEO, Future Generali India Insurance, told TOI that this is the largest cover provided by the company for any movie project. “We are not aware of other film insurance covers in India as the size of covers is not publicised. But we are sure that this is among the biggest,“ said Rao.
Future Generali has provided insurance to several big-budget movies, including Raees, Rock On 2, Dil Dhadakne Do, Mohenjo Daro and Shivaay . But all of these covers have been in the range of Rs 80-100 crore.Rao added that the company has issued 160 film insurance policies, mostly in Bollywood. “We would now like to focus on the southern market as well since we are confident of catering to the unique requirements of the film industry ,“ he said.
“Given that we have been regularly providing cover for films, we have a reinsurance treaty for this cover with GIC Re and some of the foreign reinsurers,“ said Rao. The premium rates vary for different sections.The highest rates applies to non-appearance and damage to equipment like camera where the rates can be as much as 1% of the sum insured. Other parts of the cover, such as personal accident, are much cheaper since it is for a limited period.
The film insurance policy covers risks during the preproduction to post-production stage. It insures the film against unforeseen incidents like death, illness of an actor or occurrence of natural calamities or accidental damage leading to delays in the film schedule. Additionally , it offers insurance against its legal liability to pay damages for third party civil claims arising out of bodily injury or property damage.
Cyber insurance/ Cybercrime
Introduced in 2017
Mayur Shetty, In a first, cybercrime cover for individuals, November 3, 2017: The Times of India
For the first time, individuals can buy insurance cover against cybercrime, including loss of funds to online fraud, identity theft, cyberstalking and extortion, phishing and malware attack.
While customised cyber liability cover for businesses has been around for years, these were not over-the-counter covers that could be bought by individuals. The Cyber Safe policy designed by Bajaj Allianz General Insurance is aimed at improving the level of comfort among individual internet and ecommerce users.
“This cover is the first of its kind designed keeping in mind the changing risk profile of the consumer. A couple of decades ago the biggest risk was having your pocket picked. In this day and age covers against pickpockets do not help when the bigger risk is of cybercrime,“ said Tapan Singhel, MD & CEO of the firm.
“In today's digital world, the amount of personal data being generated, transmitted, and stored on to various digital devices is growing. The critical nature of this data and the complexity of the systems that support its transmission and use have created a gamut of cyber risks,“ said Singhel. While the policy can be purchased for a sum in sured ranging from Rs 1 lakh to Rs 1 crore the company has not disclosed the premium schedule. According to officials the rate will vary depending on the number of hours the individual spends online. “The premium will be in a broad range,“ said Singhel.
The cover is not device-specific and will cover transactions made using family devices or devices at work. However, the policy expects the insured to not undertake transactions in cybercafes or suspect devices.
In addition to financial loss, the cover will compensate cost of legal defence if a hacker accesses the policyholder's credentials and puts out controversial comments in social media. Besides defending the insurer, it will also provide legal costs for proceeding against the wrongdoer in cases like stalking. Those who fall prey to sophisticated phishing frauds are also protected.
The Indian cyber insurance market is valued at Rs 30 crore only and comprises of protection bought by institutions.
Several credit card issuers have also provided cover against online fraud to cardholders.However, this protection is under a corporate cover purchased by the bank and is not available to individuals.
Disability
SC: Disabled must get benefit even when parents are alive
AmitAnand Choudhary, January 4, 2019: The Times of India
The Supreme Court on Thursday said any insurance policy taken by parents or guardians for a differently abled child should be allowed to mature after the proposer attains the age of 55 years against the present practice of giving a lump sum payment to the disabled dependent only in the event of the death of the guardian.
A bench of Justices A K Sikri, Ashok Bhushan and Abdul Nazeer said there could be “harsh cases” where disabled dependents may need payment on annuity or lump sum even during the lifetime of their parents/ guardians and asked the Centre to examine the issue.
The court also asked the legislature to consider amendments in Section 80DD of the Income Tax Act where exemption is given only to those investments made by a guardian for insurance policy, which provides payment to disabled persons only after the death of the proposer.
The court passed the order on a plea filed by differently-abled petitoner, Ravi Agrawal, who sought its direction to the Centre and LIC to allow the beneficiary of insurance policy to withdraw amount during the lifetime of parents who had taken Jeevan Aadhar policy for their children.
Flight delays
2018: cover provided

From: Mayur Shetty, Flight delayed? This policy covers spends at airport, September 13, 2018: The Times of India
New-age non-life company Digit Insurance is using data mining and analytics to develop low-cost micro products — like a cover for flight delays of 60-75 minutes — for a double-digit premium. The idea behind the flight delay policy is that passengers usually end up spending more money in the airport if they have to wait an additional hour. They will either buy a book or spend time in a coffee shop. The insurance cover compensates them by paying a claim amount of Rs 1,000.
What has enabled such a cover is technology. Given availability of flight data, the insurer can alert the buyer to claim an entitlement as soon as the flight is delayed. All the customer has to do is click on a link and upload the image of his boarding pass to receive the claim amount. According to Digit Insurance chairman Kamesh Goyal, the flight delay policy is bundled into the travel cover currently, but the company will be offering this as a stand-alone product that can be bought directly or through distributors.
The insurer’s analytics of flights has thrown up some interesting findings. The data shows that early morning flights on Tuesdays are the best option to avoid delays while those flying after 10pm on Friday are the most likely to face flight delay. Also, if you are flying out of Ludhiana, there is a one-in-five chance of your flight being delayed.
IRDAI decisions
Mental illness, adventure sports enthusiasts should be covered
Rachel Chitra, May 18, 2019: The Times of India
Insurance regulator IRDAI came out with new rules that will have widespread ramifications for health insurers and the general public. Insurers henceforth cannot decline coverage to those who have used opioids or anti-depressants. Nor can they exclude those with a history of clinical depression, personality disorders, sociopathy, psychopathy, or neurodegenerative disorders.
They cannot exclude kids suffering from development disorders such as Down’s syndrome, cerebral palsy, and autism, or those suffering from dyslexia, stammering and other disorders of speech and language. Batting for the LGBTQ community, IRDAI has said that insurers cannot discriminate on the basis of gender and identity. Insurers cannot refuse to provide coverage or reject claims if a person is on life support. Insurers can reject claims only if the patient is certified as being in a vegetative state, but even then insurers will be required to provide coverage/pay expenses till that date.
For young girls and older women who suffer from excessive bleeding, hormonal changes due to onset of puberty or menopause, insurers can no longer exclude coverage or payment for treatment costs. Insurers cannot deny coverage to geriatric patients, suffering from age-related macular degeneration (ARMD) and those suffering from rare or orphan diseases.
Insurers will have to cover adventure sports such as dirt biking, paragliding, whitewater rafting, go-karting, F1 racing, and ethnic sports like jallikattu and kambala. This would be a relief to sports enthusiasts, clubs and adventure trip organisers.
Another important decision is that at the point of claims if the person is discovered to be a smoker or suffering from a disease/pre-existing condition, the insurer cannot reject the claim if he/she has been availing of insurance for eight years in continuity.
IRDAI has said that insurers cannot exclude coverage or reject claims if the policyholder has “failed to seek or follow medical advice or follow treatment”. Often patients undergoing treatment for a condition stop the treatment towards the final stages or stop taking drugs midway. Insurers have been known to penalise patients for failure to follow through on a prescribed regime.
Health insurance/ Mediclaim: Rules, guidelines, court judgements
‘Alcohol before hospitalisation no ground for mediclaim denial’
A consumer court in Chandigarh has held that medical insurance cannot be denied just because the patient had consumed alcohol before his admission to hospital for treatment.
The forum observed that “alcohol in itself is not poison if taken in a small quantity. As it is admixture of water, sugar, and fermenting agent… if taken within limit, it cannot be said he (the complainant) was an alcoholic or it could have caused pancreatitis”.
The consumer protection panel directed New India Assurance Company to pay around Rs 1.58 lakh as medical reimbursement to complainant, Mohaliresident Sarbjit Singh Kahlon, who was denied payment on grounds that he had consumed alcohol before being hospitalised with acute abdominal pain.
Cancellation of policy must be communicated
Vasantha Kumar, Dec 19, 2022: The Times of India
Bengaluru : Unlessit is established that the insured has been informed about policy cancellation, the insurer cannot avoid the statutory liability of payment of compensation, more so in the case of third parties, the Karnataka HC has held in a recent judgment.
Allowing an appeal filed by MR Srikanta from Bengaluru, Justice HP Sandesh said the appellant/claimant is a third party whose autorickshaw hit alorry — the offending vehicle —that had abruptly stopped in the middle of the road without giving any signal around 1am on October 6,2012.
Citing the Supreme Court judgment in the Inderjit Kaur case, Justice Sandesh said the apex court had clearly held that liability for third-party risk in an insurance policy serves public interest and the same must prevail over the insurer’s interest even if the company is entitled to avoid liability for not having received the premium. The judge directed Cholamandalam MS General Insurance Company to pay Rs 2. 5 lakh as compensation to Srikanta as against Rs 1. 5 lakh with interest at 6% per annum was awarded by a tribunal.
On the contention of dishonoured cheques pertaining to the payment of premium, the judge said no documents, including the notice served upon the insured, have been produced before thecourt.
Srikanta, a resident of Guttepalya, Jayanagar, had challenged the August 25, 2014, order passed by the Motor Accident Claims Tribunal in Bengaluru. The tribunal had directed the insured — Geetha, the owner of the lorry — to pay the compensation while absolving the insurer of any liability on the grounds that the cheque issued for payment of premium had beendishonoured.
In his appeal, Srikanta claimed he had suffered a fracture of maxilla, diffuse axonal injury and right frontal sulcus subarachnoid haemorrhage, and had received treatment as an inpatient in several hospitals for 12 days.
Cannot Deny insurance to disabled
Abhinav Garg, Dec 17, 2022: The Times of India
New Delhi : People with disabilities are entitled to health insurance cover and cannot be discriminated against, Delhi High Court has said, highlighting that the right to life includes the right to health.
In a recent order, HC also directed the Insurance Regulatory and Development Authority of India (IRDAI) to remove the term “sub-standard lives” used in the rules and also to ensure such “unacceptable terminology” is not used while referring to persons with disabilities.
It was hearing a plea by an investment professional working with a hedge fund who suffered an injury in 2012 and was confined to a wheelchair due to Tetraplegia, which left him paralysed below the chest.
When he tried to obtain a health insurance policy, two insurers rejected it on the grounds of his medical condition. Justice Pratibha M Singh said people with disabilities are entitled tohealth insurance cover and cannot be discriminated against. “It is the settled position in law that the Right to Life includes the right to health and healthcare is an integral part of the same… The Rights of Persons with Disabilities Act 2016 leaves no ambiguity insofar as the entitlement of persons with disabilities for insurance. A perusal of Sections 3, 25 and 26 makes it clear that person with disabilities cannot be discriminated against insofar as healthcare and other connected aspects are concerned,” HC noted “IRDAI shall call a meeting of all insurance companies to ensure that the products are designed for persons with disabilities and other persons in terms of the circular dated June 2, 2020. The process of designing such products shall be supervised by IRDAI and it shall be ensured that the said products are introduced on an early date, preferably within two months,” the court directed. The court said irrespective of the economic standing of a person with disability, insurance coverage cannot be rejected or refused . “This court is of the opinion that there is no doubt that persons with disabilities would be entitled to health insurance coverage and products would have to be designed to enable them to obtain health insurance coverage,” Justice Singh observed.
“Refusal to issue a health insurance policy to the petitioner ought to have been a warning bell to IRDAI. Unfortunately, despite the above settled legal position and the IRDAI position on record, there is a disconnect in implementation,” it added.
Can’t debar those suffering from genetic disorders: HC
In a ruling that will benefit hapless claimants, Delhi high court has said that companies cannot deny health insurance to those suffering from genetic disorders.
Justice Pratibha M Singh held that a clause in the insurance policy excluding a person with “genetic disorder” from availing its benefit was “discriminatory” and contrary to public policy, adding that exclusion on the ground of an individual’s genetic heritage can be valid only if it is backed by rigorous and exhaustive tests.
“Right to avail health insurance is an integral part of the right to healthcare and the right to health, as recognised in Article 21 of the Constitution,” Justice Pratibha M Singh noted, upholding the decision of a trial court to decree a suit in favour of a patient who was denied medical claim on the ground of genetic disorder.
HC said exclusion of insurance claims in respect of genetic disorders creates a broad classification “which is writ with ambiguity and vagueness.”
Justice Singh further directed the Insurance Regulatory Development Authority of India to relook this exclusion clause in the insurance contracts and ensure that claims are not rejected on the basis of exclusions relating to “genetic disorders” like cardiac conditions, high blood pressure and diabetes. “The entire purpose of taking medical insurance would be defeated if all genetic disorders are excluded,” the court pointed out.
It further observed that “broad exclusion of genetic disorders is not merely a contractual issue between the insurance company and the insured, but spills into the broader canvas of right to health.” It said that “the exclusionary clause of ‘genetic disorders’ in the insurance policy, is too broad, ambiguous and discriminatory — hence violative of Article 14 of the Constitution”.
The verdict came on an insurance claim by one Jai Prakash Tayal against United India Insurance Company Limited. Tayal, who was suffering from hypertrophic obstructive cardiomyopathy, was suddenly denied his insurance claim on the ground that the said condition was genetic, and genetic diseases were not payable as per the policy.
The trial court had ruled in favour of Tayal, holding that there cannot be a discriminatory clause against persons with genetic disorders and they were entitled to medical insurance. The insurance company had appealed against the trial court’s order in August 2017.
HC took the opportunity to highlight that “citizens require a lot of effort and time to get their claims passed.” It is usual to see claimants running from pillar to post to get medical reimbursement from insurance companies, it underlined.
Can’t deny cover for HIV+ patients: IRDAI
The Insurance Regulatory and Development Authority of India (IRDAI) has said that HIV-positive individuals cannot be denied insurance cover, unless supported by actuarial studies. The regulator has asked insurers to stop discriminating against persons with HIV/AIDS.
IRDAI has made this mandatory after ‘The Human Immunodeficiency Virus (HIV) and Acquired Immunodeficiency Syndrome (AIDS) (Prevention and control) Act, 2017’ came into force from September 10. The Act bars insurance companies from discriminating against HIV-positive individuals. However, most insurance companies have stayed away from launching products for HIV/AIDS patients due to pricing-related issues.
“If the immunity is low due to a person being HIV-positive, treatment expenses go up several times. The cost of tests and duration of stay in the hospital for HIV-positive patients would be much more compared to regular patients. That is why insurance companies are wary about offering cover for persons with compromised immunity,” a senior industry official said.
New India Assurance Company CMD G Srinivasan said, “The problem is that insurers do not have enough data to design a cover for HIV-positive patients. We can offer coverage for early-stage HIV-positive patients with certain caveats and conditions.” Star Health Insurance was the first company in the country to come out with an exclusive policy for such patients on a group basis. The ‘Star Netplus Insurance Plan’ is a special policy catering to HIVpositive patients.
Can’t deny cover for several illnesses: IRDAI, 2019
Rachel Chitra , Oct 1, 2019: The Times of India
In a move that will benefit lakhs of policyholders, insurance companies have been barred from excluding illness associated with hazardous work activity, artificial life maintenance, treatment of mental illness, age-related degeneration and internal congenital diseases.
The insurance regulator said age-related ailments such as cataract surgery, knee-cap replacements, Alzheimer’s and Parkinson’s would also have to be covered. Also factory workers, working with harmful chemicals that impact health over a longterm period, can no longer be refused cover for respiratory or skin ailments that arise due to workplace conditions.
The IRDAI has also standardised exclusions, which means an insurer does not want to cover epilepsy, chronic kidney diseases and AIDS. In such cases too, there are specific wordings to be used and a specific waiting period after which coverage would begin.
Standardisation of health norms to help portability
These guidelines will greatly benefit policyholders, who disclose pre-existing conditions, as IRDAI has said, “Every health insurance product shall cover all pre-existing diseases disclosed by the persons to be insured immediately after the expiry of the 48 months waiting period or such lower period as stipulated in the product.”
Standardisation of health regulations will also help portability as the new insurer cannot set undue waiting periods. IRDAI has said, “If a person transfers from one insurer to the other — and has already completed in part some of the waiting period requirement — then the new insurer may impose only the unexpired/residual waiting period not exceeding 48 months from the date of first issuance of porting out policy.”
“Standardising of wordings of exclusions across all insurers will avoid any grey area and provide better understanding to customers. In line with medical treatments evolving and new methods coming up, insurers will be able to cover policyholders against them,” said Gurdeep Singh Batra, head (retail underwriting), Bajaj Allianz General Insurance.
But TPAs and brokers warn that while the move is pro-policyholders, it remains to be seen how it will affect pricing. “This is definitely great news for millions of people who, till now, found it difficult to obtain a cover. However, a word of caution as it might lead to a drastic increase in the premiums if insurers faced rising claims,” said Rahul Agarwal, founder, Ideal Insurance Brokers.
In November 2018, a report was submitted by a working committee to the IRDAI that insurance companies cannot exclude diseases like Alzheimer’s, Parkinson’s, HIV/AIDS and morbid obesity. This move by the IRDAI follows the recommendations of the working group.
Interest payable for delayed payment
Maha Consumer Panel Asks Insurance Co To Pay Interest To Woman
In a significant order benefitting mediclaim policyholders, Maharashtra consumer commission has held that incase there is a delay in receiving the reimbursement amount, one can claim interest on it. Ruling in favour of a woman who was reimbursed around Rs 1.7 lakh spent on an ovarian surgery almost three years after her claim, the commission said that she was entitled to 9% interest on the amount.
While New India Assurance Co Ltd had initially rejected her claim, she finally received the money in 2013 after an insurance ombudsman ruled in her favour.
Setting aside a district forum order, the Maharashtra State Consumer Disputes Redressal Commission said that it had not considered all the facts in a proper manner and wrongly came to the conclusion that the complainant had accepted the amount towards the full and final satisfaction of her claim and hence, was not entitled to get interest on that amount, along with costs and compensation.
“Opponent (New India Assurance Co Ltd) has not produced any document on record to show that complainant had received the amount towards full and final satisfaction of her claim, thus waiving her right to get interest on that amount along with costs and compensation. As she has received this amount after about three years, she is entitled to get interest on that amount,” the state consumer commission said.
The commission also ordered New India Assurance Co Ltd to pay her Rs 30,000 as compensation and costs of the complaint. The woman submitted an appeal before the state commission in 2017 after a district forum rejected her complaint in December 2016. She said that she was admitted to the hospital between April 26 and 30, 2011, and underwent ovarian surgery. She said after her claim was rejected on October 15, 2013, an insurance ombudsman ordered the insurance company to pay her the amount. In December 2013, she received the cheque from the company. She encashed the cheque.
Then, in February 2014, she gave a letter to the insurance company alleging that as her claim was given after three years, she is entitled to get interest on the amount of her claim, along with costs and compensation. When the insurance company refused this, she filed a consumer complaint.
Mediclaim covers all hospitals registered with govt: HC
Abhinav Garg & Durgesh Nandan Jha, June 13, 2019: The Times of India
In a major relief for patients, the Delhi high court has ruled that insurance companies would have to honour claims by valid medical policy holders who have received treatment at any government-registered hospital. Cashless facilities must also be extended to all such hospitals.
The court thus has put an end to a system where health insurance companies and third-party administrators (TPAs) insisted that a hospital had to be registered with them for patients to avail of insurance claims. The insurers and TPAs also dictated which hospitals could extend cashless facility.
The HC held that all patients were entitled to medical insurance, including cashless facility, as long as they held a valid medical claim policy and that the General Insurance Public Sector Association (GIPSA) — group of public sector insurance companies — could not insist that hospitals must be registered with them.
Though the current order was limited to patients seeking eye treatment, the court found fault with the very basis of GIPSA’s guidelines and the external system of “network hospitals” to exclude government-registered hospitals. It may, therefore, be applied to other treatments as well.
The order, an interim ruling, was passed by a bench of then Chief Justice Rajendra Menon and Justice Brijesh Sethi on May 31.
Plea says insurance regulator failed to keep regular checks
The HC bench specified that so long as a medical service provider is certified and registered with the state or central government, the health insurance claims of patients have to be accepted.
“We direct that till the next date of listing/ hearing, the benefit to the persons who have taken the insurance policies shall be granted strictly in accordance with the terms and conditions of the insurance policies and no other direction, order or system being followed shall be implemented till the next date,” HC said in a ruling that came on petitions filed by All India Ophthalmological Society (AIOS) and Delhi Ophthalmological Society. These organisations had filed a PIL against what they termed was the “rising influence of the insurance company and ‘TPA mafia’ within the healthcare system”.
HC further directed that “the benefit of providing cashless service be also extended to such medical health providers whose names may not be registered online with GIPSA but if they are registered with the respective state authorities as per law applicable to a particular state, the cashless service be extended even to these medical health providers/beneficiaries.”
While issuing the interim order, the HC also questioned insurance regulator IRDA on its 2018 norms that allow GIPSA and TPAs to have a network of preferred hospitals. “Issue notice to the IRDA as to why the impugned notification be not set aside and the functioning of the cartel formed by respondents be not stayed, as prima facie we observe that they have no legal status to function in the manner they are functioning,” the bench noted, asking IRDA to file its reply by next month.
It said till the next date, nursing homes and hospitals which are already registered with the Directorate of Health Services under the Delhi Nursing Home Registration Act, should not be compelled to take any further registration on the basis of the IRDA notification.
Dr Mahipal Sachdev, president-elect of the AIOS, welcomed the decision. The opthalmologists’ associations had moved HC challenging “the unauthorised parallel healthcare regulations being forced” by GIPSA, TPAs and IRDA on medical establishments.
The petitioners argued that these guidelines, compelling them to register with insurance and TPA networks, were illegal as the hospitals were already recognised by the state or central governments. They also blamed IRDA for ignoring the violations, arguing that “the influence of the insurance company and ‘TPA mafia’ within the healthcare system is so much that even IRDA is shying away from keeping regular checks on unauthorised working of these.”
Delhi Medical Association president, Dr Girish Tyagi, said they also plan to approach the court seeking universal acceptance of this order.
Health insurance/ Mediclaim, year-wise statistics
Universal Health Insurance Scheme (UHIS)
The four Public Sector General Insurance Companies have been implementing UHIS for improving health care access to poor families from the year 2003-04 onwards; The Scheme, applicable to BPL families, provides for reimbursement of medical expenses up to Rs 30,000 towards hospitalisation floated amongst the entire family; death cover due to accident for Rs 25,000/- to the earning head of the family and compensation due to loss of earning of the earning member or spouse @ Rs 50/- per cent per day upto a maximum of 15 days of hospitalization. The coverage also includes pre-existing diseases. Maternity benefits up to Rs 2,500/- for normal delivery are reimbursed and expenses for the new born are also covered. The entry into the Scheme is available for persons upto the age of 70 years.
Health expenditures rise despite insurance, not fall: 2004-14
Private Out-Of-Pocket Spending Comprises 67% Of Total Health Outgo
Increased insurance coverage in India has not led to any reduction in the numbers of those being impoverished by healthcare expenditure or `catastrophic health spending', the two main objectives of health insurance, a study has found. In fact, households with catastrophic health expenditures have risen significantly across both rural and urban India between 2004 and 2014, a time when insurance coverage rose from about 1% to 15% of the population.
This was revealed by Brookings India, a policy think tank, which brought out a report based on a study of health expenditure data from the National Sample Surveys of 2004 and 2014.
Catastrophic health expendi ture is defined as households spending over a certain proportion of their income on this head.The study considered three thresholds -15%, 25% and 40% -and the conclusion was the same in each case.
“Expansion of health insurance was a policy priority during this period and most of the increase in coverage happened because of public insurance. Yet catastrophic expenditures have risen significantly , especially for urban households. And the overall percentage of Indian households that fell below the poverty line due to out-of-pocket health expenses remained unchanged at 7% over the ten years. Is it because of the way insurance companies function or because people are unaware of what insurance coverage can provide them? We need to study why this is so,“ said Dr Shamika Ravi of Brookings India, the lead author of the report. Dr Srinath Reddy, president of the Public Health Foundation of India, pointed out that the percentage of households impoverished by health expenses remaining unchanged at 7% meant a huge increase in the number of such households (from about 77 million in 2004 to over 88 million in 2014, due to the rise in population).That's like a population larger than Germany's (just over 80 million) being pushed into poverty because of health expenses.
Dr Ravi said that increased insurance coverage appears to have increased access to hospitalised care. However, Dr Reddy pointed out that if the government was paying for the services through greater public health insurance coverage, there ought to be more accountability , without which a patient going to a private hospital could be subjected to “induced care“ and treated as an ATM.
He said hospitals tended to focus more on making money.
The study showed that private out-of-pocket expenditures comprised 67% of total health expenditure in India, which included private and government expenditure. This is one of the highest levels in the world. “What is heartening is that the OOP burden has fallen marginally in the 10 years from 2004, when it was above 70%,“ stated the study . It showed that most of the rise in out-ofpocket expenditure was due to the rise in in-patient spending and not out-patient spending.
The report also noted a “worrying“ aspect, which was that in the rural areas, out-of-pocket spending by rich has remained constant, but that by the poorest 20% has risen by 77%. This despite the poor being the target of most health insurance schemes.
The subsidy amounting to Rs 200/- for an individual, Rs 300/- for a family of five and Rs 400/- for a family of seven members is provided by the Central Government. The premium rest of subsidy Rs 100/- for individuals, Rs 150/- for a family of five and Rs 200/- only for a family of seven members.
Coverage: 2005-06/ 4.8%; 2014-15/ 28.7%
Sushmi Dey, March 5, 2017: The Times of India
Health insurance coverage in India has witnessed a sharp increase reaching 28.7% households in 2014-15 from merely 4.8% around 10 years ago, according to the latest National Family Health Survey. In fact, the penetration seems to be higher in rural areas than in urban India, making healthcare more affordable and improving health indicators. The NFHS-4 data shows 29% households in rural India have at least one member covered by a health scheme or health insurance, as compared to 28.2% in urban areas.
Expansion in India's he alth insurance coverage has helped improve various health indicators as more people are seeking treatment and medical services.
For instance, insurance penetration has resulted in significant rise in institutional deli veries reducing maternal and child mortality . Of the total deliveries, around 80% were institutional deliveries in 2014-15, up from 38.7% in 2005-06, according to NFHS-4. Though health insurance coverage continues to be driven by the government, latest data compiled by the Insurance Regulatory and Development Authority of India (IRDAI) shows Indians are increasingly buying private health insurance policies also.
According to IRDAI data, premium collected by health insurance companies during 2015-16 jumped by a 21.7% annually to Rs 24,448 crore, indicating a growing trend of people seeking coverage.
Coverage: gender-, age-wise/ 2018
May 11, 2019: The Times of India

From: May 11, 2019: The Times of India
Just 20% Indian women covered by health insurance
In India, the age group of women who face the highest average claim size is 55 and above — but this group also has the lowest number of policyholders, showing that the most vulnerable stakeholders are the least insured. As high as 60% of the policy holders fall under the age group of 26-45 years, and can be vulnerable to critical illnesses such as breast cancer, cervical cancer, vaginal cancer, etc. Of total women policy holders, as high as 75% avail of the maternity benefit. In India less than a quarter of urban, working women buy health insurance policies for themselves.
Percentage of popuation covered, city-/region- wise/ 2015
The Times of India, Mar 14, 2016
Pushpa Narayan
Chennai tops in health cover, Mumbai worst
More than half of Chennai's households have a member covered by a health scheme or health insurance. Thanks in-part to a massive government health insurance scheme that covers nearly 5 crore people, or more than three-fourth of Tamil Nadu's population, Chennai is the city with the most health-insured people among metros. Hyderabad, that comes close to Chennai, also benefits from a government insurance scheme.
Data from the National Family Health Survey -4 released by the Union health ministry shows that almost all metros have more than doubled their insured population in the past ten years, a pace organisations like World Bank say has probably not been witnessed anywhere else in the world.
In Chennai, 56.8% of households are covered by health insurance followed by Hyderabad with 49.8% and Kolkata with 26.1%. Among the metros, Mumbai (city) has the lowest coverage at 12.4%. The data for New Delhi, however, is yet to be released.
Among states, more than three-fifth of the people in TN got health insurance in the last decade, lowering the number of uninsured by 60% from 2005-2006. At the national level, 17% of the population was under the health net until 2014.
Experts link the leap in numbers to the state-sponsored health insurance schemes in TN, Kerala, Telangana, Andhra Pradesh, Karnataka and Maharashtra. The climb began when a state-sponsored scheme was launched by the DMK government in July 2009, two years after the AP government launched its Arogyashri. In 2012, the AIADMK regime upgraded the scheme and extended its coverage to include some 1.5 crore families.
While state insurance is available to the poor, many in the middle and upper-income group now have a company-sponsored insurance or an individual insurance. "Today, even if a few of the private insurers aren't making huge profits, their losses are down," says Star Health Insurance CMD V Jagannathan.
The TN scheme is offered through the United India Insurance Company Ltd, a public-sector undertaking headquartered in Chennai. The scheme provides free medical and surgical treatment for up to Rs1.5 lakh in government and private hospitals to the members of any family whose annual family income is less than Rs.72,000.
Between January 2012 and March 2016, the scheme has paid Rs 29 billion towards 14 lakh claims. Most people were allowed to be treated in private hospitals that have been empanelled under the state scheme. "This is beside the free treatment we roll out at government hospitals, some of which earned money through this scheme. It was used for development works such as air-conditioning wards, buying better drugs, equipment and improve housekeeping services at hospitals," said Dr J Mohanasundram, former dean of Government General Hospital.
24% growth in 2016-17, highest ever
Rachel Chitra, Health cover biz ends FY17 on record high, April 21, 2017: The Times of India

Increasing incidences of lifestyle-related health complications and rising medical expenditure have propelled the health insurance industry to its best ever year. Data from the Insurance Regulatory and Development Authority of India (IRDAI) shows health cover business grew nearly 24% year-on-year to Rs 30,765 crore for 2016-17, compared with 22.4% growth in 2015-16 and 15.6% growth in 2014-15.
In the last three years, the sector -which constitutes over 24% of the general insurance industry -has been on a high-growth curve. “The main reason why people are buying more insurance is medical inflation. The cost of medical treatment is growing 10-15% year on-year in India. More people are realising the need for it -many fall into a debt trap once impacted.
Just look at the most common diseases like cardiac ailments. A simple angiography costs Rs 35,000, an angioplasty will cost Rs 2-3 lakh and an open heart surgery (CPAG) upwards of Rs 5 lakh. So while medical treatment expenses are rising, people's salaries aren't. Hence, the necessity for medical insurance,“ said Puneet Sahni, head (product development), SBI General Insurance.
“Another reason for growth is that salaried employees find that their corporate group health cover does not cover all ailments. To cope with rising medical expenses, working class individuals are going for individual health covers or top-ups on existing corporate group mediclaim policies,“ said Sahni. Standalone health insurers are witnessing rapid growth at more than 40%, ahead of private insurers growing at just over 15% and the four PSUs at 23%.

From: Rema Nagarajan & Rachel Chitra, Sharp hike in health insurance premium hits senior citizens, December 24, 2017: The Times of India

From: Rema Nagarajan & Rachel Chitra, Sharp hike in health insurance premium hits senior citizens, December 24, 2017: The Times of India
No-Claim Bonus Scrapped; Cos Cite Rising Losses
Kolkata-based Mr and Mrs Soubito Banerjee, who are in their 70s, saw their medical insurance premium almost double from Rs 32,000 to Rs 63,000. Chennai-based Annathai Gopalakrishnan (68) will pay Rs 58,000, up from Rs 29,000. In general, a health insurance cover of just Rs 5 lakh for a 65-year-old couple now costs Rs 84,000 per annum, as against Rs 54,000 five years ago.
For many senior citizens living on a pension, the increase is stiff. At their age they cannot switch to another insurer, and a switch is pointless because the companies have raised rates in tandem.
One big reason for the increase is the withdrawal of the 15% discount on the premium for no claims. There was also a family discount of 10%, available to at least two members seeking cover. Together, that accounted for a significant 25% discount on the premium. These discounts were stopped by insurance companies last year after IRDA ruled in 2013 that those who had made a claim could not be charged higher premiums.
Though the discounts have been withdrawn for everyone, seniors take a larger hit because premiums rise with age. “My client has been paying insurance premium for more than 30 years. He used to be careful, paying small hospital bills from his own pocket to maintain the no-claim status,” a health insurance agent told TOI. That strategy will no longer work. G Srinivasan, CMD of New India Assurance Company, says insurers face losses of 300% in the senior citizen category. “The primary cause is medical inflation. Hospitals have no regulator, but we do. We are forced to increase prices for our viability.”
‘Group insurance to cos priciest segment’
Another reason is that IRDA allows us to increase prices only once every three years. Our last price revision was in 2012,” added Srinivasan, “We’d still be making losses in this (senior citizen) portfolio. We’d have to increase the prices even more drastically if we want to break even.”
V R Sehgal (name changed) is a worried man. The 57-year-old pays Rs 43,500 per annum for the Rs 5 lakh health cover he bought for himself and his wife 25 years ago. After retirement, when his income will fall to Rs 20,000 per month, he will need to pay about Rs 60,000 per annum till the age of 65, and more than Rs 84,000 afterwards.
Data from Insurance Regulatory and Development Authority (IRDA) shows group health insurance provided to businesses is the most expensive segment for insurers (see graphic).
Corporate employees’ claims actually amount to more than what they pay as premiums while individual insurance payers claim the least.
2013-16: The limited benefits of health insurance policies
Rema Nagarajan, September 12, 2018: The Times of India

From: Rema Nagarajan, September 12, 2018: The Times of India
Individual buyers of health insurance are worst off in India, especially if they have bought it from private stand-alone health insurance companies. They have the greatest difficulty in getting the companies to pay up when they need the cover.
The Indian health insurance sector also had the highest complaints rate, according a study of the sector that compared India, Canada, Australia, UK and the US state of California, an indication of the poor quality of products and services.The study concluded that “it may be the case that with such poor levels of consumer protection, households which purchase basic financial products, like health insurance, are worse off than households which do not”.
According to the study by the National Institute of Public Finance and Policy (NIPFP) titled Fair Play in Indian Health Insurance, the claims ratio or the amount paid to settle claims as a percentage of the total premiums collected had fallen from 67% to 58% between 2013 and 2016 for private standalone health insurers, raising consumer protection concerns. Yet, unlike in the US, a highly privatised health insurance market, where it is mandatory for insurers to refund consumers if the claims ratio is below a minimum level, no such provision exists in India. In many US states the minimum claims ratio ranges from 65% to 80%, below which insurers would have to refund consumers.
In contrast, the claims ratio of government-backed general insurance firms had gone up from 106% in 2013-14 to 117% in 2015-16, indicating either a cross-subsidy from other businesses or a business heading towards bankruptcy. The study also found that private insurers use a higher percentage (up from 10% in 2013-14 to over 12% in 2015-16) of the premium paid by consumers to pay agent commissions, while public sector insurers used just 6.8% in 2013 and now over 7% for the same.
The largest growth in the sector was in the governmentfunded health insurance schemes (GFHIS), which went from covering 12% of the population in 2013-14 to over 20% by 2015-16. These enable the poor to use private hospitals for covered medical procedures and the insurer reimburses the private hospital. Group health insurance, like those offered by companies to their employees, and individual insurance covered just over 4% and 2%, respectively, of the population. The authors noted that with private persons buying health insurance, and governments building state-funded schemes that use the services of private health insurance firms on a large scale, there was an urgent need to look into the quality of these insurance policies and efficiency of the sector.
In computing complaint rates, the study only considered complaints made to adjudicators outside the company, which indicated that the company had failed to address the consumer’s grievance. Moreover, in most other countries since clinical visits, medication and some wellness care are also covered, and not just hospitalisation, there were more chances for customer dissatisfaction. Despite there being fewer encounters between consumers and insurance firms in India, as they cover only hospitalisation, and being a far less litigious country, India has the highest complaint rate. “The lack of fair play in this industry is derived from deficiencies in regulations, weak enforcement and faulty institutional design of consumer redress,” noted the study.
Insurance firms often rejected legitimate claims only to lose in dispute resolution mechanisms, like the ombudsman and consumer fora. There are no penalties in the existing regulations for rejecting valid claims even when the rejections are in violation of the regulations, the study noted, adding that firms violated regulatory requirements without any repercussions. “In multiple cases, after more than a year of dispute resolution processes, the insurer is required to pay for the insured amount and small values for litigation costs and harassment damages. Usually the costs imposed are even below the time value of the claimed amount,” the study said, noting how rejection of legitimate claims helped further insurance firms’ surplus.
Unlike in US, where it is mandatory for insurers to refund consumers if the claims ratio is below a minimum level, no such provision exists in India. In many US states, the minimum claims ratio ranges from 65% to 80%, below which insurers would have to refund consumers Insurance firms often reject legitimate claims only to lose in dispute resolution mechanisms... There are no penalties in the existing regulations for rejecting valid claims even when the rejections are in violation of the regulations.
2015: a system fragmented over several insurers

From: Nov 29, 2019: The Times of India
See graphic:
Health Insurance in India, vis-à-vis similar countries, 2017
2018, Health policies to cover mental illness
Rachel Chitra, Health policies to cover mental illness, August 17, 2018: The Times of India

From: Rachel Chitra, Health policies to cover mental illness, August 17, 2018: The Times of India
IRDAI Asks Insurers To Immediately Comply With New Mental Health Law
Insurance regulator IRDAI on Thursday issued a circular directing insurers to cover mental illness, which has reached serious proportions in the country.
The Mental Healthcare Act, 2017 — which came into force from May 29 — has made it mandatory to provide “for medical insurance for treatment of mental illness on the same basis as is available for treatment of physical illness”. But to date, none of India’s 33 insurers has introduced a product that covers ailments such as depression, schizophrenia, and bipolar disorder, even though such covers are commonplace in many countries.
The IRDAI order says, “All insurance companies are hereby directed to comply with the...provisions of the Mental Healthcare Act, 2017 with immediate effect.”
Health insurance firm Cigna TTK’s COO Jyoti Punja described it as a progressive step. “This will ensure a life of dignity to those who have mental health issues. We believe it will create awareness, acceptance, and inclusion of mental illness as any other physical ailment. It will ‘normalise’ diagnoses, by reducing associated myths and stigma,” Punja said.
Activists and psychiatrists feel the change has been long overdue. Dr Soumitra Pathare, psychiatrist and director at the Pune-based Indian Law Society’s Centre for Mental Health Law and Policy, said, “It is extremely inhuman to discriminate people in this fashion. Today, no one can say we won’t cover cancer, tuberculosis or heart attack. So why do we have this block towards covering mental health issues? They are just as debilitating and corrosive to a person’s well-being as physical ailments.”
Mental health conditions have always been in the list of exclusions of health insurance policies. The only exceptions to this have been the coverage of development conditions such as autism and Down’s syndrome by the National Health Insurance Scheme, and a few private schemes like Star Health Insurance’s cover for autistic children.
Companies wishing to include mental health coverage will have to file a fresh product with the IRDAI, or add this to an existing product and file again. “They have to revise the rates, look at the actuarial risk, increase premium if need be. So far, no insurance company has filed for such a change with the regulator,” said a government official.
Star Health Insurance executive director Dr S Prakash said there is a spectrum of disorders. “At the lower end you have anxiety and depression. At the upper end there’s obsessive compulsive disorder, bipolar, borderline narcissistic personality disorder. We should first cover the lower end. It does seem harsh to tell a person we can’t cover you, when they are already depressed,” he said.
ICICI Lombard General Insurance chief actuarial officer Sanjay Datta said it is a question of actuarial and financial risk. “It is uncharted territory. There are two coverages needed: First, OPD cover for therapy, consultation and drugs. Second, hospitalisation or rehab, which would be long-term and expensive. In western countries, both are covered. But in India, it is untested ground,” he said.
2019/ ‘Insurance must cover MRI, pre-operation expenses’
Rebecca Samervel, January 7, 2019: The Times of India
If you pay from your pocket for tests before a surgery, you are entitled to a refund from your mediclaim insurance company. This order favouring policy holders was passed recently by the state consumer commission. This includes expenses on an MRI scan done a month prior to the surgery, says the order. The consumer commission also specified that expenses incurred on consultation and pre-surgery tests cannot be refused just because the policy holder had spent the amount 30 days before the surgery.
The commission brought to book New India Assurance Company Limited for having rejected a reimbursement claim made by a Dombivli resident, V Sridhar. It pertained to pre-surgery and non-medical expense (gloves for medical use) incurred for his son’s knee surgery.
Sridhar’s son had been hospitalised on April 18, 2012. While Sridhar had claimed Rs 58,000, the insurance company approved around Rs 49,000. The commission’s order states that the company will now have to pay the entire claim of Rs 58,000 along with Rs 35,000 as compensation.
In his complaint, Sridhar had stated that the mediclaim policy covered his son, wife and himself for Rs 1 lakh. The complaint said that when he first submitted his claim, the company had agreed to honour it only to the extent of Rs 17,852. Sridhar said that when he made inquiries, the company agreed to reimburse Rs 30,856, but refused to compensate for expenses prior to hospitalisation and non-medical expenses.
2019/ Reveal ailment before policy is issued

From: Rebecca Samervel, For insurance claim, reveal ailment before policy is issued, December 20, 2018: The Times of India
The state consumer commission has clarified that a person who takes an insurance policy must inform the company of any health issues that crop up right from the date she hands in a filled-out proposal form till the policy is issued.
The commission recently dismissed a complaint a Mulund-based man had filed against an insurance company when it rejected the Rs 5 lakh life cover claim after his wife’s death from cancer in 2013. The insurer said the woman had suppressed crucial information about the illness when she submitted the proposal form, but her husband contended that she was diagnosed only after the policy proposal was submitted.
Insurance policy was issued after cancer diagnosis: State commission
The commission, though, pointed out that the policy was issued only a week later and it was incumbent upon the woman to inform the insurance company about the cancer during the intervening week.
“Although the wife of the complainant learnt on July 22, 2011, that she was suffering from cancer of the oesophagus, she had not informed this fact to the insurance company till issuance of the insurance policy in her favour (July 30, 2011). Under such circumstances, we are of the opinion that the wife of the complainant had suppressed material facts in respect of her health before the insurance company had issued insurance policy in her favour,” said the state commission.
The complainant had moved the Maharashtra State Consumer Disputes Redressal Commission in 2016 after a district forum rejected his plea against Life Insurance Corporation of India.
The commission said the forum had rightly considered the facts and reached the conclusion that the insurance company had rightly repudiated the claim.
In his appeal, the man had told the commission that his wife had taken two policies of Rs 2.5 lakh each. He said his wife had submitted the proposal form on July 20, 2011. He further said that two days later, his wife was admitted to a hospital where she was diagnosed with cancer. She died on March 16, 2013. The man then submitted his claim to the insurance company but it was repudiated. He moved the district forum in 2015.
After going through the relevant documents, the state consumer commission found that the woman had signed the policy proposal form only on July 22, 2011, the same day that she was admitted to the hospital and her cancer diagnosed.
2019/ ‘Tobacco not sole reason for cancer, insurer must pay’
January 10, 2019: The Times of India
A consumer court in Ahmedabad ordered insurance companies to pay the claim for a policyholder’s cancer treatment with the observation that chewing tobacco cannot be considered the only cause for oral cancer. The complainant, Kanaiyalal Modi, smoked and chewed tobacco for the last four years.
The Consumer Dispute Redressal Forum, Ahmedabad city, asked New India Assurance Co Ltd and Health India TPA Services Pvt Ltd to pay Modi Rs 1.12 lakh, which he had spent on his surgery for oral cancer in December 2014.
The court held that the rejection of his claim was improper and was a deficiency in service and unfair trade practice. It ordered the insurance companies to pay him Rs 3,000 extra as compensation for mental harassment and legal expenditure.
The court said, “It cannot be believed that cancer was caused solely because of his habit of chewing tobacco. His claim should have been accepted. It is a clear deficiency in service and unfair trade practice on the part of the opponents.”
After being treated at an oncology centre, Modi made a claim for the sum. The companies rejected it citing the treating doctor’s certificate and clinical history. These revealed that Modi habitually used chewing tobacco and this was a breach of the policy conditions.
Modi argued that the doctor’s certificate showed his tobacco habits, but it also mentioned that the habit could not be considered the sole reason for his cancer. The court said his cancer was not a pre-existing disease as Modi had held the policy since 2003. It acknowledged that the doctor’s certificate revealed tobacco use habits, but the certificate also said the “exact reason for oral cancer cannot be determined”.
Smoker can’t be denied mediclaim for cancer
Saeed Khan, Oct 2, 2021: The Times of India
A consumer court has ordered an insurance company to reimburse the expenditure on medical treatment for lung cancer after the company refused mediclaim on the grounds that the patient was a chain smoker and contracted cancer due to his smoking. The consumer court said there was no proof that the cancer had been caused by the patient’s smoking habit.
The case involved one Alok Kumar Banerjee, who underwent treatment for adenocarcinoma of the lung from Vedanta Institute of Medical Science in July 2014 and incurred a medical bill of Rs 93,297. He had medical insurance cover. But his claim was rejected by the insurer. After Banerjee passed away, his widow Smita sued the insurer in 2016 in the Consumer Dispute Redressal Commission, Ahmedabad (additional).
‘Discharge summary can’t be primary proof’
The insurance company took the defence that Banerjee was treated in different hospitals for his illness, which had a direct nexus with his smoking habit, and that this was reflected in his case papers. The consumer commission did not agree. It cited a higher forum’s order and said that a discharge summary itself cannot be treated as primary or conclusive evidence in the absence of any independent proof. There was no evidence in this case to show that the patient got cancer because of smoking.
The insurance company’s doctor gave a medical opinion that those who smoke have a 26 times higher risk of getting cancer. To this, the commission said that merely on the basis of this opinion it cannot be concluded that the patient got cancer due to smoking.
Those who do not smoke also get lung cancer and it cannot be believed that all those who smoke have lung cancer. It cannot be accepted that the complainant’s husband got cancer because of his smoking habit and the insurer had wrongly rejected the claim, the commission added.
2022-24: The major ailments, claim size
Mayur Shetty, August 10, 2024: The Times of India
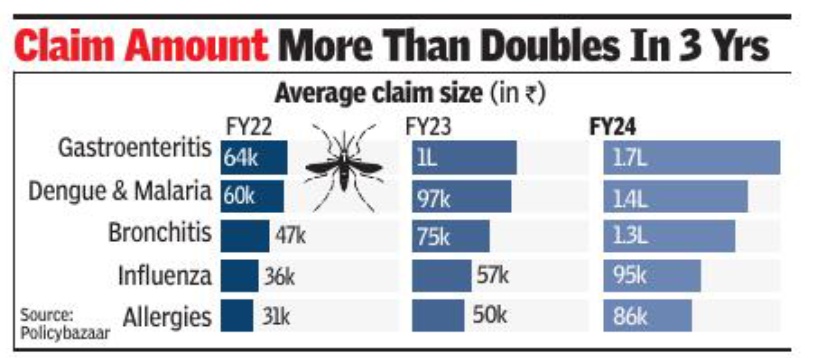
From: Mayur Shetty, August 10, 2024: The Times of India
Mumbai : Nearly a third of the health insurance claims recorded by insurers are due to seasonal infectious diseases. These include vectorborne diseases such as dengue and malaria, which give rise to high claims in July and August, or water-borne infections such as gastroenteritis. In winter, it is usually bronchitis or influenza.
As many of these claims are related to hygiene conditions in the locality they are avoidable to a large extent. However, they impact all segments of society as evident from claims data.
According to a study of reported health insurance claims by Policybazaar, vector borne diseases like Dengue and Malaria account for 15% of total seasonal illnesses claims. The cost for treating these mosquito borne diseases typically ranges from Rs 50,000 to Rs 1,50,000. These claims surge in July and August when humid conditions create ideal breeding grounds for mosquitoes.
Another illness that peaks during the monsoon is gastroenteritis or stomach flu which has the same treatment expenses as Malaria. This ailment accounts for 18% of seasonal claims. Another 10% of seasonal illness claims are due to allergic reactions where the periodicity varies according to region. Winter sees claims due to influenza and bron- chitis peaking to 20% and 12% of seasonal illnesses. However, the cost of treatment is lower ranging from Rs 25,000 to Rs 1 lakh.
“If you look at developed countries, the share of seasonal illnesses is much lower compared to developing countries. In case of India, even in developed parts of the country like Gurgaon there are problems of water accumulation and mosquito breeding which leads to an increase in these cla- ims,” said Siddharth Singhal, head of health insurance, Policybazaar.
“These seasonal illnesses add to the frequency of claims. However, the average claim amount is much lower than chronic illnesses, and in terms of value, the share of claims would be below 20%,” said Singhal.
According to Singhal, the cases of hospitalisation for illnesses that would have earlier been treated at home have gone up. “This is a positive development as it is always good to have professional support. This leads to reduction in mortalities,” he said. Policybazaar is the largest online distributor of insurance and the claims data includes those of its own customers as well as those obtained from other health insurance providers
Nuclear Operator's Liability Policy, 2016
The policy
The Times of India, May 27 2016
1st N-power cover to push pvt investments
Mayur Shetty
The country's first Nuclear Operator's Liability Policy has been issued to Nuclear Power Corporation of India, underwritten by a consortium of insurance companies through the India Nuclear Insurance Pool. The policy was the missing component from the set of requirements for getting private investment in nuclear power --the doors for which were opened ten years ago when the then Manmohan Singh-led government signed the civil nuclear agreement with the US.
The entire Rs 1,500-crore India Nuclear Insurance Pool is entirely supported by domestic companies and is managed by General Insurance Corporation (GIC), which has also committed funds to the pool. The first policy was issued by New India Assurance -the largest state-owned company .
Alice Vaidyan, chairperson, GIC, said, “In all history , there have been only three nuclear accidents -Three Mile Island (US), Chernobyl (now Ukraine) and Fukushima (Japan). The probability of an incident is extremely low . But the incidents are very severe.“ Although the nuclear deal ended India's isolation, investment was not forthcoming. This was because nuclear risks are generally excluded by insurers and nuclear power operators have a maximum liability of Rs 1,500 crore under the new law.
Profits
2016: 1 of 22 makes underwriting profits
The Times of India, Aug 25 2016
Mayur Shetty
Only 1 of 22 non-life insurers makes underwriting profits The insurance regulator's proposal to force companies to list might have come at an inopportune time for non-life companies. As many as 21out of the 22 non-life insurers continue to lose money in the main insurance business. Bajaj Allianz General Insurance has emerged as the only non-life company to make underwriting profits among the 22. The JV between Bajaj Finserv and German insurer Allianz also tops the list of private insurers in terms of net profits with post-tax earnings of Rs 564 crore. It also ranks No. 2 in terms of premium income and has the highest return on equity at 20.2%.
Typically, companies make underwriting losses as they cut rates to grow business. But Bajaj Allianz has turned out to be an outlier. “In the last five years, we have grown our premium at a compounded annual growth rate of 65%. This shows that there is no trade-off between growth and underwriting profits,“ said Tapan Singhel, MD & CEO, Bajaj Allianz.
To improve governance, the Insurance Regulatory and Development Authority of India (IRDAI) has proposed mandatory listing for insurance companies after a decade of operations. There are 16 life in surers, 12 non-life companies, one health insurer and two specialised insurance companies which have been around for more than a decade.
While companies have reached maturity , underwriting profits are yet to emerge for most of them. The high level of underwriting losses could be a damper for investors, although companies report net profits because of the investment income earned from their reserves.
PSU insurers post losses in H1FY17
Rachel Chitra, PSU insurers post losses in H1FY17 on higher claims, Jan 2, 2017: The Times of India
Public sector insurers such as United India and Oriental Insurance have posted losses for the first half of 2016-17, faced with higher claims, operating costs and an aggressive sales strategy . Solvency margins -a key indicator of a company's profitability and ability to settle claims -also raised red flags. Solvency ratios of National Insurance (1.26) and Oriental (1.14) were well below the regulator's statuary requirements of 1.50, even as some top private players had an average ratio of 2.53.
Many private players such as Future Generali, Bharati Axa General, Kotak Mahindra, Star Health and Cigna TTK also posted significant losses.Their loss before tax for the first half of 2016-17 was Rs 11.86 crore, Rs 19.09 crore, Rs 15.82 crore, Rs 71.58 crore and Rs 82.34 crore respectively.
“The large public-sector giants are faced with different issues. But for young private players, they need to balance growth with profitability and solvency margins. One can't deplete capital reserves. We are an industry that operates on unpredictability -catastrophes, terrorism, natural disasters. We have to keep our solvency at certain levels so that we can fulfil the trust policyholders repose in us to pay claims,“ said Sanjay Datta, chief (underwriting & claims), ICICI Lombard General Insurance.
Another problem is overcompetition among insurers for the same business without increasing insurance penetration. India's general insurance industry's penetration levels are at an abysmal 0.72%, according to sector regulator Irdai's 2015-16 annual report. All four public-sector giants had massive underwriting losses for the half year -New India's underwriting loss was Rs 1,803 crore, followed by United at Rs 1,533 crore, Oriental at Rs 1,465 crore and National at Rs 991 crore. While New India's large base and position as the No. 1insurer in India account for its large underwriting losses, its more prudent underwriting practise and solvency margin of 2.04% is a benchmark that its other public-sector peers have not been able to meet.
“Sustained underwriting losses for the general insuran ce industry implies that insurers are too preoccupied in the pricing game to look beyond upping their capabilities to focus on improving the customer experience and may also eventually impact the services offered,“ said Tapan Singhel, MD and CEO, Bajaj Allianz General Insurance Co. Insurers said that the mart has seen several new ent ket has seen several new entrants, intensifying competition by focusing only on growth which has led to competitive pricing pressure.
Growth at what cost? This is a question private insurers are trying to answer by scaling back, after rapid growth and a fierce price war between 29 general insurers hammered down the industry's collective profits. Top private insurers ICICI Lombard (8.88% from 9.23%) and Bajaj Allianz (5.71% from 6.10%) saw their marketshare dip between September to November 2016.
2017: 32% Growth, half of it from Crop insurance
Mayur Shetty, Crop insurance drives non-life biz , April 14, 2017: The Times of India

Industry Grows 32% In FY17, Touches `1L-Cr For 1st Time
Crop insurance has helped the non-life industry record 32% growth the last fiscal and cross the Rs 1-lakh-crore mark for the first time. From nowhere, crop insurance has emerged the third largest line of business after motor insurance and health insurance following the launch of the Pradhan Mantri Fasal Bima Yojana (PMFBY) last year .
Business figures for nonlife insurance companies released by the Insurance Regulatory and Development Authority of India (IRDAI) for the year 2016-17 show that total premium income jumped to Rs 1.27 lakh crore from Rs 96,376 crore in FY16. Usually, the growth in the non-life segment reflects the growth in the real economy, new investments and sale of automobiles. This year, the industry has managed to re cord its highest growth since liberalisation, despite absence of any new projects, due to the opening up of crop insurance.
“Of the 32% growth, nearly 16% came from crop insurance,“ said G Srinivasan, chairman, New India Assurance, the country's largest insurer. He added that business would be good for the topline as well as crop loss claims were expected to be around 75% of the premium. While the year has been good for farmers, Karnataka and Tamil Nadu saw crop damage due to drought. Bhargav Dasgupta, MD & CEO, ICICI Lombard General Insurance, the largest private insurer, said, “For us, crop insurance is almost 10% of total premium and it's the third biggest line of business.“
This is the first year that there is a completely marketdriven crop insurance scheme. The earlier National Agriculture Insurance Scheme (NAIS) was primarily a government programme and administered by the Agriculture Insurance Corporation of India. Under the PMFBY, insurers quote market rates. However, the farmer pays only 2 percentage points of the sum insured as premium and the rest is subsidised by the government.
Dasgupta said, “We have gone in for reinsurance as the severity of claims can be extremely high and loss ratios (ratio of claims to premium) can go up to 200%.“ He said that next year the premium from crop insurance would be higher as the penetration is set to increase from present level of 28%. The value of the total crop insured during the current financial year would be in the region of Rs 3 lakh crore.
Besides providing cover, non-life companies aim to reduce losses by roping in weather companies and providing advice to farmers on the risks involved. According to figures released by the insurance regulator, the four public sector non-life companies -New India Assurance, National Insurance, Oriental Insurance and United India Insurance -continue to retain the top slots. However, they have grown slower than the industry at 24% and marginally lost market share.
2017: 1 of 21 makes underwriting profits

Bajaj Allianz continues to be the only company to report an underwriting profit during FY17 with all other companies paying out more by way of claims than they earn as premium. The company has also emerged as the most profitable private general insurer. The underwriting results refer to the income from the primary business of insurance. Despite 20 of 21 general insurers reporting underwriting losses, 16 companies still reported a net profit due to investment income.
Most insurers say that given the relatively higher returns in fixed-income investments in India, companies can function with a marginal underwriting loss. Non-life companies have an opportu nity to earn from the substantial reserves they are required to maintain. Non-life companies at any time have substantial reserves as they are required to collect premium upfront and they pay claims over a period of time.
Another parameter used for measuring the efficiency of a company is the combined ratio (CoR). This is the ratio of claims plus operating expenses to the total premium income. For Bajaj Allianz, the combined ratio is 96.8% as against 121.3% for the industry . The industry ratio is dragged down by public sector companies and smaller general insurance companies. Oriental Insurance in the public sector has the highest ratio of 148%, while Liberty Videocon and Kotak Mahindra in the private sector have a ratio of 146%.
Bajaj Allianz General Insurance MD & CEO Tapan Singhel said, “We are a strong retail company . Margins are better in retail if you do it sensibly . We focus on the customer so that he or she is ready to pay the right price.“ According to Singhel, there is no business segment that the company keeps out of in order to avoid underwriting losses. “Our market share in motor, health and crop insurance is in line with our overall market share of 7%. We even do group health insurance business,“ said Singhel.
2018: no disasters, non-life cos. see higher margins
Mayur Shetty, With no disasters, non-life cos see higher margins, June 2, 2018: The Times of India

Underwriting results
From: Mayur Shetty, With no disasters, non-life cos see higher margins, June 2, 2018: The Times of India
See graphic:
FY18 profit after tax;
Underwriting results
Three Insurers Report Underwriting Profits
In a pointer to improved margins in the general insurance industry, three non-life companies have reported underwriting profits as against only one last year. Underwriting losses — excess of claims paid over premium — have narrowed for most companies, indicating that prices have firmed up for corporate insurance space. Industry numbers for FY18 show that Bajaj Allianz continues to be the most profitable general insurer and has improved margins further.
According to data released by non-life companies in their public disclosures, three have generated underwriting profits — Bajaj Allianz General Insurance (Rs 293 crore), Universal Sompo (Rs 290 crore) and SBI General (Rs 94 crore). Bajaj Allianz is also the most profitable non-life company in the private sector with a net profit of Rs 921 crore — an increase of 26% over the net profit in the previous year.
Bajaj Allianz General Insurance MD & CEO Tapan Singhel said, “Last year, the industry had no major catastrophe. This has an impact of 5-6% on the overall margins. In the past, we have seen floods cause widespread losses on motor portfolio.” Another factor that has improved bottom lines, according to Singhel, was the listing of insurance companies, which has shifted focus to margins. The companies that listed in FY18 are New India Assurance, ICICI Lombard and national reinsurer GIC Re.
However, the non-life industry is extremely cyclical and improved margins often lead to more aggression for market share, which leads to pricing coming under pressure. “We have already seen prices coming under pressure during April renewals,” said Singhel.
The largest private non-life company ICICI Lombard General Insurance reported a profit of Rs 862 crore — an increase of 22% over previous year. The company has also narrowed its underwriting loss to Rs 231 crore from Rs 318 crore in FY17.
2017-18, Net profit, loss of non-life industry
Mayur Shetty, IP Os boost prof its of non-life cos, August 16, 2018: The Times of India

From: Mayur Shetty, IP Os boost prof its of non-life cos, August 16, 2018: The Times of India
The non-life industry has reported a remarkable turnaround with net profits of Rs 6,465 crore for the year ended March 2018 as against Rs 160 crore in the previous year. The turnaround is despite the Kolkatabased National Insurance Company reporting a record loss of Rs 2,171 crore.
The huge loss by National notwithstanding, stateowned insurers reported a net profit of Rs 2,543 crore for FY19 as compared to a loss of Rs 2,550 crore in FY17. One of the reasons for improvement in profits appears to be the promoters’ decision to list the companies. During the year, the largest public sector insurer New India Assurance and the largest private insurer ICICI Lombard General Insurance got listed on the stock exchanges following an initial public offer.
Bajaj Allianz General Insurance (BAGIC) continues to be the only insurance company to report underwriting profits in the non-life industry. The company has maintained its combined ratio at 92.3% in 2017-18 as against 96.8% in 2016-17 — the lowest in the general insurance industry. The combined ratio is the percentage of the total premium income to cost of incurred claims and management expenditure. The company’s MD & CEO Tapan Singhel said, “In FY18, there has not been any major catastrophic event. Also, prices were better for some business like fire. And group mediclaim business saw an improvement in margins too. This year, there has been a softening of prices.”
In FY18, BAGIC posted the highest underwriting profit of Rs 293 crore as compared to Rs 64 crore in 2016-17. According to Singhel, BAGIC has managed to beat the trend because of its focus on retaining underwriting margins. “We believe that customers should come to us because they see value — we do not play the price game,” said Singhel.
The improvement in the performance of the public sector was driven by New India Assurance, which doubled its net profit to Rs 2,201 crore from Rs 1,008 crore in FY17. The other two public sector insurers Oriental Insurance and United India also reported net profits of Rs 1,003 crore and Rs 1,510 crore in FY18 as against losses of Rs 1,912 and Rs 1,691 crore in FY17. The improved profits were on the back of better underwriting results (difference between the premium collected and claims incurred). National’s underwriting losses, however, worsened from Rs 3,680 crore to Rs 5,600 crore in FY19.
2018-19: 3 PSUs drag industry into red
Mayur Shetty, August 12, 2019: The Times of India

From: Mayur Shetty, August 12, 2019: The Times of India
Three public sector insurance companies have dragged down the non-life industry into a Rs 44-crore loss in FY19. National, Oriental Insurance and United India have together reported losses of Rs 4,200 crore, which is more than the collective profits of the remaining 23 companies. The three unlisted state-owned insurers were the last to announce their financial results. The government is eyeing a merger and a subsequent listing of these companies. However, due to their poor financial performance, they will require a capital infusion. The performance of the PSU insurers in FY19 is in sharp contrast to their financials in FY18.
In FY18, the four PSU insurers — including the listed New India Assurance — reported a combined net profit of Rs 2,543 crore. This, taken with the private industry’s profits of Rs 3,922 crore, translated into a Rs 6,341-crore profit for the industry in that year. In FY19, the four PSU insurers reported a combined loss of Rs 3,628 crore despite New India turning in a Rs 645-crore profit.
The private insurers have reported a net profit of Rs 3,584 crore — a drop of 8%. Industry officials say that profits have declined partially because the industry did very well in crop insurance in the previous year, which was not the case in the year under review. Also, underwriting losses in property insurance have been very high, prompting the General Insurance Corporation to hike rates in some segments.
The reason for the poor performance of the PSU companies is their huge underwriting loss (see graphic), which is the excess of claims over premium. In India, most insurers do report underwriting losses but make up for it through investment income. This is because premium is required to be collected up front and companies earn interest or investment income on them. In FY19, only Bajaj Allianz, Universal Sompo and SBI General reported underwriting profits of Rs 18 crore, Rs 43 crore and Rs 82 crore respectively.
The PSU insurers reported an underwriting loss of Rs 18,490 crore — a 47% increase over the Rs 12,507-crore loss in FY18. The private industry also saw underwriting losses jump 62% to Rs 2,864 crore from Rs 1,762 crore in the previous year. However, since the margins of the private companies were better, they still managed to turn in better profits.
Senior citizens' insurance
`Only 1.6% elderly have health cover'
Sushmi Dey,
December 06 2014
Less than two of every 100 senior citizens in India are covered under public and private health insurance. This even as the population of elderly people is growing significantly and is forecast to hit almost 300 million in around two decades. The elderly population, aged more than 60 years, is projected to constitute 18.3% of the total population in 2050, up from 7.7% in 2010, according to the United Nations. Their population will grow to 112 million by 2015 from 72 million in 2000.
However, health insurance penetration among this population remains significantly low in India. A recent study by Deloitte shows mere ly 1.6% of elderly population is covered under public and private insurance schemes.“This low insurance penetration amongst the elderly is fur ther exacerbated by inadequate coverage provided to the insured, in terms of both amount and type of services covered,“ the report states. Experts point out the overall health insurance penetration in India is as it is low at 26%, as compared to other countries. According to World Bank estimates, India's healthcare spending as a percentage of GDP is among the lowest in emerging markets.During 2012; India spent a total of around 4% of GDP on healthcare, whereas Brazil and China spent 9.3% and 5.4%, respectively.
Currently, there is a lack of emphasis on insurance cover for the elderly . Most private players do not want to cover the elderly in their plans because the expenditures are high as compared to premiums earned, experts say.
Social media insurance
2018: companies show interest
Rachel Chitra, Cos rush for social media insurance, August 4, 2018: The Times of India
The rising wave of intolerance in India is pushing organisations to ensure their insurance policies cover the fallouts of social media hate or unintentional corporate goof-ups. Insurers say companies fear litigation and expenses in the event of incidents such as when a DDI World employee tweeted a hate message against Kashmiris, or when a Kotak Mahindra Bank employee justified the Kathua rape.
Organisations are insisting on new and more comprehensive clauses in their normal professional indemnity and directors & officers’ (D&O) liability insurance policies. Some insurers even offer specialised covers such as ICICI Lombard General Insurance’s media liability cover and Bajaj Allianz General Insurance’s cyber safe policy. These include social media liability.
The D&O liability insurance coverage seeks to protect individuals from personal losses if they are sued as a result of serving as a director or an officer of a business or other types of organisation.
ICICI Lombard General Insurance chief underwriting officer Sanjay Datta said, “Awareness has been increasing. For corporates, managing possible reputational risk and litigation is important. When the Satyam fraud issue happened, there was an immediate uptick in D&O policies.”
Datta said companies need to take policies that are comprehensive as they face a wide range of risks — it could be a matter related to comments on social media, it could be about religious discrimination, gender wage gap, company results, company policy, or employee dissatisfaction. “Company executives, independent or working directors, and board members could get sued by shareholders, employees or the public,” he said.
In the case of Kotak Mahindra, it had quickly fired the employee for making the Kathua rape comments.
Media firms more exposed to content related issues
Dutta said, “Employees can sue, citing wrongful termination. They can sue both the corporate entity and the management, which is where the D&O policy would kick in.” Public sector insurers say older policies can handle such fallouts of social media without the need for a special cover.
“Social media liability insurance may be a new concept with the rising popularity of LinkedIn, Twitter and Facebook. But it basically is a take-off on traditional covers,” said an official of United India Insurance Company.
SBI General Insurance head (product development) Puneet Sahni said media companies, in particular, have wide exposure to such content-related issues and take more comprehensive covers. Indians are seen to be getting easily offended, as in the case of Priya Warrier’s wink video that went viral.
“Media companies run the risk of getting sued for inappropriate content or what people find inappropriate — on content related to religion, gender, identity, ethnicity or sexual preferences. It may be a subjective matter, but there is still the litigation to be faced and costs to be borne,” said Sahni.
Organisations are insisting on new and more comprehensive clauses in their normal professional indemnity and directors & officers’ liability insurance covers
Theft insurance
No claim on cover if no violence: SC
The Times of India, Aug 24 2016
Dhananjay Mahapatra
The Supreme Court ruled that for someone to claim compensation from an insurance company for burglary , the theft has to be accompanied by forced entry , violence or threat of violence. A bench of Justices A R Dave and L Nageswara Rao held that words used in an insurance policy agreement were sacrosanct and could not be diluted to mean anything other than what was stated in the document.The bench said that it could not substitute words which were not intended. The Supreme Court has ruled that a person or an entity can't seek compensation on insured goods if theft happened without violence. Citing a 2004 SC judgment, Justice Rao said, “In the absence of violence or force, the insured cannot claim indemnification against the insurance company. The terms of the policy have to be construed as it is and we cannot add or subtract something.Howsoever liberally we may construe the policy , we cannot take liberalism to the extent of substituting the words which are not intended.
“...in common parlance, the term `burglary' would mean theft but it has to be preceded with force or violence. If the element of force or violence is not present, then the insured cannot claim compensation.“ The ruling came in case where an Odisha PSU had claimed insurance amount of Rs 34.40 lakh in addition to the cost of litigation it incurred by fighting its case till the apex court.
Industrial Promotion and Investment Corporation of Orissa, a public sector undertaking, had advanced a loan of Rs 40.74 lakh to Josna Casting Centre Orissa Pvt Ltd. On default of repayment, the PSU took over the assets of the private company and insured its assets in 1996 for Rs 46 lakh under `burglary and housebreaking policy' with New India Assurance Company.
The seized assets were put to auction in January 1997 and it was detected that some parts of the plant and machinery were missing from the factory premises. An FIR was registered in Remona police station, Balasore, regarding theft of the machinery .
The PSU lodged an insurance claim for an amount of Rs 34.40 lakh under `burglary and housebreaking policy'.The insurance firm rejected the claim saying theft did not come under the purview of the policy as there was no evidence to show someone had forcibly broken into the factory premises or threatened employees before making away with the goods. The bench dismissed the PSU's petition.
Travel insurance not popular
Singh, Only 30% of those who bought e-tickets opted for insurance, Nov 21 2016 : The Times of India
Out of the 410 tickets booked on the IRCTC website -accounting for 695 passengers of the ill-fated Indore-Patna express -only 126 (accounting for 209 passengers) included the recently announced travel insurance that costs less than Re 1.
TOI has learnt that those travelling on 78 (128 passengers) of the 126 tickets are eligible for the insurance payout. The other passengers who opted for insurance cover were to board the train from Kanpur onwards.
The IRCTC website offers passengers the option of availing of travel insurance at a premium of 92 paise. The scheme was announced by Union railway minister Suresh Prabhu in his budget speech. The scheme offers compensation of Rs 10 lakh in the event of death or total disability , Rs 7.5 lakh for partial disability , up to Rs 2 lakh for hospitalisation expenses, and Rs 10,000 for the transportation of a passenger's mortal remains from the accident site or any other untoward incident -terrorist attack, dacoity , rioting, or arson.
The facility is available to passengers who book the eticket, excluding for suburban trains, irrespective of the class of the ticket. The option to buy the insurance cover is available through a checkbox. “The premium is just 92 paise, so lack of awareness or sheer negligence while booking tickets may be the reason why so many passengers failed to opt for insurance,“ an official said.
See also
Insurance, life and general: India
Insurance (general): India